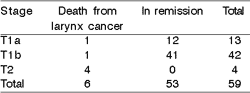Year: 2002 Vol. 68 Ed. 5 - (12º)
Artigo Original
Pages: 673 to 677
Oncologic results of the partial laryngectomy for early glottic carcinoma
Author(s):
Otávio Alberto Curioni 1,
Marcos Brasilino de Carvalho 1,
Josias de Andrade Sobrinho 1,
Abrão Rapoport 2
Keywords: glottic carcinoma, partial laryngectomy, results.
Abstract:
Introduction: The squamous cell carcinoma of the larynx is the sixth most common neoplasia, being the the second neoplasia of the head and neck, immediately after oral cancer. Depending of the stage of lesion, extension of the cancer at diagnosis, there is a quite favorable long term prognosis, with global survival rate for 5 years of 65%-70%. Aim: Evaluation of the results after partial laringectomy for early glottic squamous cell carcinoma. Study design: Clinical retrospective. Material and Method: Retrospective analysis of the 59 patients' handbook was accomplished submitted to the partial laringectomy. There were excluded patients with previous treatment, tumor extension larger than 10 mm below the glottis, lesions with macroscopic extension for vestibular folds and lesions with decrease of the mobility vocal cords laryngoscopy and follow-up of 36 months or more. Results: 12 patients (20,3%) presented recurrence, being 1 a regional recurrence (1,7%) and 11 local recurrences (18,6%), with surgical rescue (total laringectomy) and oncologic control in 75% of those cases. Severe complications (glottic stenosis and aspiration) happened in only 2 patients (3,4%). Conclusions: The partial laringectomy is safe and an effective procedure for the treatment of majority of early glottic carcinoma. In addition, for its versatility, check safety in the oncologic radically and make possible, also, the functional readaptation for the patient
![]()
INTRODUCTION
The squamous cell carcinoma of larynx is ranked in 6th place among the most common neoplasms, and is one of the most common malignant diseases of head and neck ranking in second place right after cancer of the oral cavity.1. Generally, the disease affects middle age and elderly men that are smokers. Depending on staging of the lesion, or on cancer size at diagnosis, long-term outcome is highly favorable with a 5-year overall survival rate of 65% to 70% of the patients2.
Obviously, therapeutic evaluation depends mainly on the primary lesion site and size, which is evaluated by indirect or direct laryngoscopy, and imaging tests. Other additional examinations include clinical exam and neck palpation to measure direct invasion or lymphonode metastasis, full physical examination to detect distant metastasis and hystopathological analysis of biopsy samples.
Although high frequency radiation has achieved outstanding safety level of functional and oncologic results 3,4 and precision techniques with stringent indications for functional surgery of the larynx have been providing a fully competitive outlook in terms of management options available to head and neck surgeons over the last years, open surgery and external radiation remain key strategies to treat squamous cell carcinoma of the larynx. Still, indications did not achieve consensus due to the lack of randomized studies comparing effectiveness of both treatments5. Generally, radiation therapy or surgery is considered for all T1 and T2 cancers, most of the T3 and T4 need multimode therapy, typically associated with additional radiotherapy5, 6. On the other hand, some factors might have relative impact in therapy's choice, namely patient's age, use of voice professionally, uncontrolled smoking and drinking habits, and some social-economic factors that might demand short-term treatment. Certainly, the objective is to cure cancer with minimal dysfunction and maximum quality of life after treatment and with the highest likelihood of cure possible. In case of tumors in early stage (T1 and T2) there is already a common sense stating that partial excision of certain larynx compartments is compatible with cure and presents proper functional outcomes 7.
Conventionally, in the Head and Neck Department of Heliopolis Hospital, Hosphel, in Sao Paulo, the two management practices are significant, however, surgery indications are prevalent not only in advanced lesion, but in those tumors considered initial (T1 and T2) as well. Based on this surgical experience, this study proposed the analysis of oncologic control-related results in 59 patients with T1/T2 glottis carcinoma that have undergone partial laryngectomy, in addition to the analysis of rescue rate after recurrence against the literature. This study was evaluated and approved by the Ethical Committed under the # 131 protocol.
MATERIAL AND METHOD
Retrospective analysis of the chart of 59 patients that have undergone partial laryngectomy and results of epidemiological characteristics such as age, smoking and drinking habits, in addition to the clinical /endoscopy exam of the site, kind of surgery performed, treatment results and hystopathological analysis.
Previous requirement to take part in the study were as follows: T1 or T2 squamous cell carcinoma not previously treated (UICC-1997); tumor size above 10 mm below the glottis, macroscopic lesions for vestibular folds; lesions with vocal folds gross mobility decrease in indirect laryngoscopy and patients with follow up below 36 months.
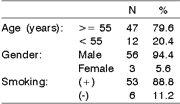
In reference to epidemiological characteristics, 56 patients were male (94.4%) and 3 female (5.6%), 47 were above 60 (79.6%) and 12 (20.4%) were under it, 53 were smokers and 6 were not (Table 1). In terms of clinical staging for inclusion in the study, 57 cases were T1 stage (22 T1a and 35 T1b) and only 2 cases were T2 stage (Table 2). The analysis of surgical findings evidenced higher number of T1b cases (42), 13 T1a cases, and 4 T2 cases (Table 3).
In recurrent patients, an attempt to correlate the primary lesion size, type of surgery, local recurrence and treatment provided was made. (Table 5).
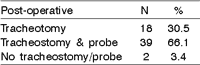
The distribution of the patients that needed tracheostomy and post-operative enteral probe, and re-adapted and non-adapted patients (patients that recovered voice and swallowing without probe/tracheostomy, and those patients that need it) are respectively described in Table 6 and 7.
Table 8 describes patient's status until last appointment after the rescue treatment, with evidence of unfavorable outcome for T2 tumors.
RESULTS
As to extension of the disease, surgical findings confirmed by hystopathological exam described high number of cases with anterior commissure involvement (Table 3), and fronto-lateral laryngectomy was the most used technique (Table 4).
Clinical characteristics and surgery findings of the 12 recurrence cases were confronted for location, initial lesion, staging, recurrence site, and rescue treatment against the patients' outcome (Table 5). The bimodal recurrence trend was found in cases of recurrence within the first postoperative year, and after 30 months. This would suggest a behavior compatible with second primary lesion.
Tracheostomy was performed in 57 patients (96.6%) and enteral probe was used in 39 patients (66.1%), tracheostomy and enteral probe were not used in only in 2 cases (3.4%) (Table 6). Only two patients did not readapt (3.4%), one suffered tracheobronchial aspiration and withdrawal of enteral probe could not be achieved, and the other could not have the canulla removed due to glottic stenosis (Table 7).Table 1. Clinical- epidemiological characteristics of the population
N is the number of patients (59)
Table 2. Tumor distribution according to T pre-operative stage
N is the number of patients (59)
Table 3. Tumor distribution according to second T-surgical stage
N is the number of patients (59)
Table 4. Patient distribution according to the type of surgery
LFL = Fronto-lateral laryngectomy ; HL= emilaryngectomy;
LSC=Supra-cricoid laryngectomy
N is the number of patients (59)
Table 5. Patients that needed new treatment due to recurrence
LFL= Fronto-lateral laryngectomy; HL= Hemilaryngectomy; LSC= Supra-cricoid laryngectomy;
LT= Total laryngectomy; FL= Pharyngolaryngectomy; MOCA= Death due to cancer; VSD= Alive in remission; PV = vocal fold.
N = Twelve cases of recurrence after partial laryngectomy
Table 6. Patient distribution according to post-operative use of tracheostomy and enteral probe
N is the number of patients (59)
Table 7. Patient distribution according to postoperative adaptation (without enteral probe & tracheostomy)
N is the number of patients (59)
Table 8. Patient evolution according to T surgical classification
DISCUSSION
Local control is clearly the most important prognostic factor of stage I and II glottic cancer, since local and distant metastasis are only rarely found in the absence of local recurrence in such patients8,9. Therefore, all efforts should be made in curative treatment to achieve increased cure rates with sparing of laryngeal functions. These goals could be achieved with partial laryngectomy with low complication rates (approximately 10%). The most common were glottic stenosis, tracheobronchial aspiration; granulomas and poor vocal quality. Functional and control outcomes accounted for 95% and 80% of the T1 and T2 tumors, respectively10,11. In this study only 2 patients had severe complications (1 case of glottic stenosis, and 1 of tracheobronchial aspiration) (Table 6).
In T1 glottic tumors both surgery and radiation were accepted to provide similar oncologic control, especially if we consider that a failures leads to rescue surgery12,13. Open surgery is recommended for T1b and T2 stage glottic tumors, but some authors advocate endoscopic resection for such stages14, 15. The justification for using open surgery in T1b tumors, in which the rule is to have the anterior commissure involvement (it occurs only in 30% of T1a tumors) is the significant reduction of disease control reported due to radiation or surgery, with higher recurrence rate than in any other site of the larynx16,17. This behavior could be explained by the fact that laryngeal mucosa is very close to the thyroid cartilage and the neoplasm could infiltrate into the vocal ligament fibers and through blood vessels and penetrate in the cricothyroid cartilage and membrane. This infiltration is more resistant to radiation and is removed by surgery. T2 glottic tumors form a heterogeneous group of lesions with distinct results reported in the literature for both surgical and radiation therapy, and control rates ranged approximately from 80% and 55% to 75%, respectively, if rescue surgeries were not taken into account.
In the patients studied, fronto-lateral laryngectomy was the minor surgery most frequently performed to treat several tumors with anterior commissure involvement. Cases in which tumor content accounted for more than 2/3 of the vocal fold and were close to the anterior commissure were considered unfavorable for minor procedures.
Twelve (12) (20.3%) out of 59 cases reported recurrence, and were initially considered regional recurrence (1.7%) and 11 were local recurrence (18.6%). Four (4) out of those 12 patients 4/59 (6.8%) had recurrence 55 months after the surgery. These tumors could represent a second primary tumor, since two (2) occurred in the opposite vocal fold (patients 7 and 9) and two (2) occurred in the hypopharynx and supraglottis (patients 5 and 6). Cases of recurrence on the 12 month after surgery were attributed to poor microscopic oncologic margin in which recurrences occurred in areas juxtaposed with the resection (patients 1, 3, 4, 8, 10, 11, 12). The other case was a late cervical recurrence whose local extension was into the supraglottis, characterizing a potentially more aggressive tumor with increased likelihood of therapeutic failure (patient 2), and was not viewed as local treatment failure. In reference to local recurrence of partial laryngectomy, the literature reported that the option in most of the cases is the rescue with total laryngectomy, in which disease control could be achieved in 60% of re-operated cases. 19,20 In our material, total laryngectomy performed to rescue provided disease control in 75% of patients (6/8). The analysis of total recurrence rate and control likelihood with surgical rescue showed that this rate dropped approximately 55% (6/11). It could be explained by the patient's profile of this institution. Many patients could not maintain desired follow up regularity due to social-economic and/or cultural factors and presented advanced recurrent disease when they came back making the new treatment unfeasible.
The outcomes reported that open laryngectomy is an excellent therapeutic procedure for selected patients with initial lesions of the glottis, particularly with anterior commissure involvement, and are similar to those found in the literature19,20. In this study, T2 glottic tumors had unfavorable response to the surgery performed with 3 local recurrences reported. (Table 8) The first-year recurrences after treatment were probably due to both supraglottis invasion, which is not commonly found in this region 18,12, and improper microscopic surgical margin. The other recurrences that occurred after the 4rth-postoperative year, which characterize bimodal distribution of recurrences in our sample, suggested that they were second primary neoplasm. Stringent pre-operative evaluation is essential for accurate surgical indication, as well as for the social profile, since it may affect disease control rates in the long term.
CONCLUSION
Partial laryngectomy is a safe and effective procedure to treat most of the early stage glottic cancers. In addition to its versatility, that provides safety to radical oncologic disease and it also allows functional re-adaptation of the patients.
REFERENCES
1. Vokes EE, Weichselbaum RR, Lippman SM et al. Head and neck cancer. N England J Med 1993;328:184-194.
2. Gallo A, Vicentiis M, Marciocco V, Simorelli, M, Fiorella ML, Shah JP. CO2 Laser cordectomy for early-stage glottic carcinoma. A long-term follow-up of 156 cases. Laryngoscope 2002;112:370-374.
3. Shah JP, Karnell LH, Hoffman HT et al. Patterns of care for cancer of the larynx in the United States. Arch Otolaryngol Head Neck Surg 1997;123:475-483.
4. O'Sullivan B, Mackillop W, Gilbert R et al. Controversies in the management of laryngeal cancer: results of an international survey of patterns of care. Radiother Oncol 1994;31:23-32.
5. Smith MC, Goffinet DR. Radiotherapy for CIS of glottic larynx. Int J Radiat Oncol Biol Phys 1994;28:251-255.
6. Small W Jr, Mittal BB, Brand WN et al. Role of radiation therapy in the management of carcinoma in situ of the larynx. Laryngoscope 1993;103:663-667.
7. Carvalho MB. Tratamento cirúrgico dos tumores malignos da laringe. In: Carvalho MB. Tratado de Cirurgia de Cabeça e Pescoço e Otorrinolaringologia. 1a ed. São Paulo: Atheneu; 2001. p. 927-939.
8. Olsen KD, Thomas JV, DeSanto LW, Suman VJ. Indications and results of cordectomy for early glottic carcinoma. Otolaryngol Head Neck Surg 1993;108:277-282.
9. Olsen KD, Thomas JV, DeSanto LW, Suman VJ. Early glottic carcinoma treated with open laryngeal procedures. Arch Otolaryngol Head Neck Surg 1994;120:264-268.
10. Biller HF, Ogura JH, Pratt LL. Hemilaryngectomy for T2 glottic cancer. Arch Otolaryngol 1971;93:238-242.
11. Ogura Jh, Biller HF. Elective neck dissection for pharyngeal and laryngeal cancers. Ann Otol Rhinol Laryngol 1971;80:646-651.
12. Mendenhall WM, Parsons JT, Springer SP, et l. T1-T2 vocal cord carcinoma: a basis for comparing the results of radiotherapy and surgery. Head Neck Surg 1998;10:373-377.
13. Rothfield RE, Johnson JT, Myers EN, et al. Hemilaryngectomy for salvage radiation therapy failures. Otolaryngol Head Neck Surg 1990;103:792-793.
14. Davis RK. Transoral laser surgery for glottic cancer. Adv Otorhinolaryngol 1995;49:254-258.
15. Davis K, Kelly S, Stevens M. Selective management of early glottic cancer. Laryngoscope 1990;100:306-9.
16. Kirchner JA. What have whole organ sections contributed to the treatment of laryngeal cancer? Ann Otol Rhinol Laryngol 1989;98:661-667.
17. Rucci L, Gammarota L, Gallo O. Carcinoma of the anterior commissure of the larynx: II. proposal of a new staging system. Ann Otol Rhinol Laryngol 1996;105:391-396.
18. Harwood AR, Deboer G. Prognostic factors in T2 glottic cancer. Cancer 1980;45:991-995.
19. Pontes PAL, Brasil OC. Controvérsias acerca do tratamento do câncer glótico. In Carvalho MB. Tratado de Cirurgia de Cabeça e Pescoço e Otorrinolaringologia. 1ª ed. São Paulo: Atheneu; 2001. p 961-968.
20. Monhr RM, Quennelle DJ, Shumrick DA. Vertico-frontolateral laryngectomy. Indications, technique and results. Arch Otolaryngol 1983;109:384-395.
1 Assistant Physician, Department of Head and Neck Surgery and Otorhinolaryngology, Hospital Heliópolis, Hosphel. São Paulo, Brazil.
2 Coordinator of the Post-Graduation Course in Head and Neck, Hospital Heliópolis, São Paulo/SP.
Study conducted by the Department of Head and Neck Surgery and Otorhinolaryngology, Hospital Heliópolis, Hosphel, São Paulo, Brazil.
Address correspondence to: Prof. Dr. Abrão Rapoport - Rua Iramaia, 136 Jd. Europa 01450-020 São Paulo
Tel. (55 11) 289-6229/ 287-4347 - E-mail: cpgcp.hosphel@attglobal.net
Article submitted on April 25, 2002. Article accepted on August 8, 2002