Year: 2004 Vol. 70 Ed. 2 - (18º)
Relato de Caso
Pages: 265 to 267
Jugular phlebectasia in children: a case report
Author(s):
Raquel C. de Oliveira 1,
Claudiane M. Assis 2,
Alexandre R. Coraçari 3,
Fernando D. Molina 4,
José Victor Maniglia 5
Keywords: phlebectasia, children, jugular vein.
Abstract:
Neck masses that appear only on straining are rare in children and should be differentiated between laryngoceles, superior mediastinal tumors or cysts and jugular phlebectasia. The latter being an abnormal fusiform or saccular dilatation of the jugular vein. We report a case of external jugular phlebectasia in a healthy child. A variety of ethiological hypotheses have been proposed: anatomic abnormality of the vein, mechanical compression of the brachiocephalic vein, acquired lesion of the vein and idiopathic. Most patients are asymptomatic, the diagnosis can be established clinically and confirmed by imaging studies. Conservative or surgery management will be chosen according to the symptoms.
![]()
INTRODUCTION
Neck masses in childhood that are manifested only during physical exercise are rare and the main differential diagnoses to be made are laryngoceles, cyst or upper mediastinum tumor and jugular phlebectasia 1, 2. Jugular phlebectasia is a saccular or spindle abnormal dilatation of the jugular vein that was described for the first time in 1875 by Harris3, according to the British literature. After the 70's, as a result of non-invasive diagnostic methods and the increased number of neck and laryngeal surgeries performed, this medical entity has been frequently recognized. Over 100 cases of phlebectasia involving the neck veins, including internal, external and anterior jugular veins have been described in the world literature. Even though many names have been proposed, the most widely accepted term in phlebectasia 4, which indicates dilation without tortuous aspect, differentiating it from varicose veins. We reported the case of external jugular vein phlebectasia in a healthy child.
CASE REPORT
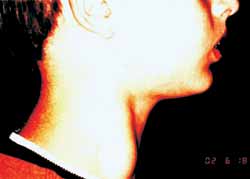
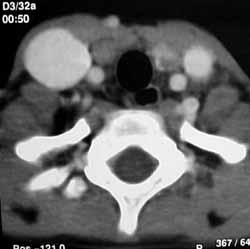
T.H.T., 10-year-old male Caucasian patient, presented complaint of right neck mass for one year, visible only after physical exercise, without history of fever, neck trauma, weight loss, anorexia or other complaints. The physical examination presented neck mass on the medium third of the anterior margin of the sternocleidomastoid muscle on the left, 3x2cm, visible with Valsalva's maneuver, of elastic consistency, mobile, non-painful, without local phlogistic signs or pulsation (Photo 1). Neck computed tomography (CT) revealed dilation of internal jugular vein on the right without compression of adjacent structures (Photo 2). Since the patient remained asymptomatic and without increase of mass during the six-month follow-up, no invasive procedure has been indicated.
DISCUSSION
Many hypotheses have been proposed to explain the etiology of jugular phlebectasia, among them anatomical abnormalities of the vein caused by congenital wall structural defect, mechanical compression of brachiocephalic vein between the head of the clavicle and the right lung apex, and acquired and idiopathic vein lesions 2. The histopathological study of jugular vein walls clearly indicates reduction of elasticity of venous wall caused by loss of elastic tissue and hypertrophy of connective tissue, narrowing of venous wall, fibrosis and absence or reduction of smooth muscle cell layer. The intermittent increase of intrathoracic pressure associated with the changes described above play an important role as causal factor, despite the absence of literature reports of venous flow obstruction 4.
Jugular phlebectasia is more common on the right side, probably owing to the most lateral location of the right brachicephalic vein and its relation with other veins at the sternoclavicular junction and by direct contact with lung pleura on the right. Therefore, insuflation of right lung apex leads to sufficient increase of pressure of brachicephalic vein to produce obstruction and temporary distension of jugular vein 5. There are more rare cases of bilateral and left jugular phlebectasia.
Normally, it is an asymptomatic condition, but some patients can complain of tightening sensation, suffocation or vertigo, discomfort during physical activity, swallowing and cough, lingual pain and aphony when speaking loud 2.
The diagnosis can be defined based on strong clinical suspicion, being confirmed by ultrasound with Doppler6,7, CT scan 8,9, venography 10 or arteriography 11.
Asymptomatic patients should be followed up clinically in view of complications such as thrombosis 12 and Horner's syndrome 13, which are rare, and rupture, which had not been reported, whereas symptomatic patients should be submitted to surgical excision. The symptomatic cases with bilateral impairment are a challenge for surgeons to choose which side to operate on. Some authors advocate surgery in asymptomatic cases considering the tendency of growth and the possible esthetical deformity 1, 2, 4, 5.
CLOSING REMARKS
Despite being rare, jugular phlebectasia should be included in the differential diagnosis of neck masses in childhood, especially when related to Valsalva's maneuver. Since it is a benign condition, in which symptomatology is scarce and complications are rare, we advocate conservative management, reserving surgery only for specific cases.
Photo 1. Right profile.
Photo 2. Axial CT scan of neck region.
REFERENCES
1. Reed JA, Grewal H. Jugular phlebectasia manifesting as an unusual neck mass in a child. Am J Surg 2001; 182: 289-90.
2. Sander S, Eliçevik M, Ünal M, Vural O. Jugular Phlebectasia in children: Is It Rare or Ignored? J Pediatr Surg 1999; 34(12): 1829-32.
3. Harris RI. Congenital venous cyst of the mediastinum. Ann Surg 1928; 88:953-6.
4. Paleri V, Gopalakrishnan S. Jugular phlebectasia: theory of pathogenesis and review of literature. Int J Pediatr Otorhinolaryngol 2001; 57:155-9.
5. Nwako FA, Agugua NEN, Udeh CA, Osuorji RI. Jugular Phlebectasia. J Pediatr Surg 1989; 24(3): 303-5.
6. Shimuzu M, Takagi Y, Yoshio H, Takeda R, Matsui O. Usefulness of ultrasonography and Doppler color flow imaging in the diagnosis of internal jugular phlebectasia Heart vessels 1992; 7: 95-8.
7. Walsh RM, Lannigan FJ, McGlashan JA, et al. Jugular bulb phlebectasia Int J Pediatr Otorhinolaryngol 1993; 25: 249-54.
8. Balik E, Erdener A, Taneli C et al. Jugular phlebectasia in children. Eur J Pediatr Surg 1993; 3: 46-7.
9. Walsh RM, Murty GE, Bradley PJ. Bilateral internal jugular phlebectasia. J Laryngol Otol 1992; 106: 753-4.
10. Yashiro N, Lio H. Internal jugular phlebectasia in children Radiat Med 1984; 2: 136-9.
11. Passariello R, Cozzi F, Casalena G, Colarossi G, Rossi P, Simonetti G. Angiographic diagnosis of jugular venous system dilatation in children Report of 5 cases. Radiology 1979; 8: 247-50.
12. Spiro SA, Coccaro SF, Bogucki E. Aneurysm of the internal jugular vein manifesting after prolonged positive pressure ventilation Head Neck 1991; 13: 450-2.
13. Inci S, Bertan V, Kansu T, Cila A. Horne's Syndrome due to jugular venous ectasia. Childs Nerv Syst 1995; 11: 533-5.
1 Resident Physician, Department of Otorhinolaryngology and Head and Neck Surgery, FAMERP.
2 Resident Physician, Service of Otorhinolaryngology and Head and Neck Surgery. Clínica Maniglia.
3 Resident Physician, Department of Otorhinolaryngology and Head and Neck Surgery, FAMERP.
4 Physician, Responsible for the Service of Pediatric Otorhinolaryngology, Department of Otorhinolaryngology and Head and Neck Surgery, FAMERP.
5 General Director, FAMERP, Head of the Discipline of Otorhinolaryngology and Head and Neck Surgery, FAMERP.
Address correspondence to: Claudiane Mozer de Assis, Rua Ondina n 45 Redentora São José do Rio Preto SP 15015-200
E-mail: clauorl@yahoo.com.br
Presented at 36 Congresso Brasileiro de Otorrinolaringologia, November 19 - 23, Florianopolis, SC.