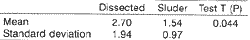Year: 2001 Vol. 67 Ed. 3 - (4º)
Artigos Originais
Pages: 319 to 324
Tonsillectomy: Dissected x Sluder.
Author(s):
Edson C. M. Monteiro*,
Fabiana M. N. Rocha**,
Erika Y. Ikeda**,
Cátia M. R. Lemes***,
Giovana P. Dall'Oglio****.
Keywords: tonsillectomy, conventional dissection, Sluder's guillotine
Abstract:
Introduction: The tonsyllectomy by Sluder technique hasn't been used for many complications in the present. The aim of this study was to compare the morbidity in Sluder and conventional dissection technique. Study design: Clinical prospective. Material and method: We studied a hundred children with hypertrophics tonsills who underwent a tonsyllectomy by conventional dissection and Sluder tecnique, where was made a questionary. Results: The Sluder technique had a minor surgical time and bleeding than conventional dissection technique. The post-operative analysis proved better clinic recovery in the Sluder technique. Conclusion: We concluded that both techniques are resolutive however the Sluder technique suggested statically minor morbidity.
![]()
INTRODUCTION
Resection surgeries of palatine tonsils and adenoids, especially those indicated in adenotonsillar hypertrophy, leading to impairment of breathing in children, are ancient procedures and restricted to few techniques5,6,11,13,14. In recent years, authors have frequently employed traditional dissection by detachment, putting aside the technique described by Sluder.
According to some authors, in the eight published volumes of Medical Encyclopedia, dated the year 3 AD, Cornelius Caesus provided one of the first descriptions of tonsifectomy9. The most common procedure is dissection by traditional method13, and most recently, by laser.
Tonsillectomy using Sluder tonsillectome is no longer a used technique because of clinical risks unfairly imputed to the surgery, which were partly caused by anesthetic procedures. We performed a comparative study between Sluder's technique and traditional dissection, under general anesthesia and with orotracheal intubation, in order to analyze morbidity comparing both procedures.
MATERIAL AND METHOD
Between November 1997 and June 1998, we studied children who underwent adenotonsillectomy in the age range from 4 to 8 years. The surgical indication was due to upper respiratory obstruction affections caused by adenoid and tonsil hypertrophy.
Selected cases were submitted to nasofibroscopy to confirm enlargement of adenoids. Next, we checked the need for adenotonsillectomy and not only tonsillectomy.
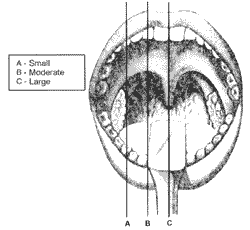
Classification of size of palatine tonsils
Size of palatine tonsils was classified according to the following criteria (Figure 1):
A - Small - tonsils aligned with the palatoglossal folds (anterior pillar);
B -Moderate - projection of tonsils between palatoglossal folds (anterior pillar) and midline (uvula);
C -Large - tonsils reach the midline that goes through the uvula.
In our study, we selected cases that had palatine tonsil hypertrophy classified as large.
We subdivided the subjects into two groups:
Group 1 - conventional dissection (50 cases);
Group 2 - dissection with Sluder guillotine (50 cases).
We also designed a protocol that was filled in by the responsible surgeon.
Figure 1. Classification of size of tonsils.
Criteria for evaluation of method
The study involved more than 100 patients but we selected only those that met the criteria determined for the study (protocol). The cases included actually came to post-operative visits. Cases not followed during the postoperative period were excluded from the sample.
The surgical time was counted as from the moment the mouth opener was introduced, until its final removal. Blood losses were measured in milliliters found in the aspiration tube.
In the comparative study we used two statistical tests: independent t test (for numerical information) and quisquare test (for categorized information). In the independent t test (p), we considered statistically significant difference if p was equal or below 0.05. In the qui-square test, we considered statistically significant difference if the value observed was equal or below the critical value.
Description of conventional dissection method
The patient was positioned at Rose's position, under general anesthesia with Halothane (halogen anesthetic) and orotracheal intubation, placing Mc'Ivor mouth opener and gauze anchored on the hypophatynx.
After visualization, the tonsils were pulled medially with a Brunnings' clamp, perpendicular to the pillar. Pharyngeal mucosa was incised at the level of the anterior pillar (Figure 2), with a knife number 12, from the lingual fold up to the posterior pole. We looked for the tonsil capsule, and using Hurd's aspirator-detacher (Figure 3), we released the tonsil from the lateral wall of pharynx with cranio-caudal firm movements, reaching the inferior pole until complete exeresis of the tonsil (Figure 4). Alternatively, we cut the tonsil pedicle using Metzembaum curved scissors (Figure 5). Next, we made hemostasis with gauze and, if necessary, we sutured with simple catgut 2-0. The same procedure was followed on the other side.
Figure 2. Incision of pharyngeal mucosa at the level of anterior pillar.
Figure 3. Dissection of tonsillar capsule.
Figure 4. Detachment of tonsil from the inferior pole.
Figure 5. Exeresis of tonsil.
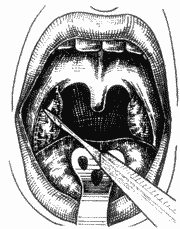
Figure 6. Placement of tonsil (inferior pole) in Sluder's guillotine.
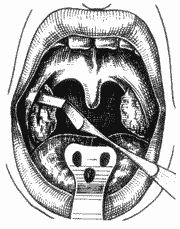
Figure 7. Pressure of anterior pillar with the indicator finger of the opposite hand.
Description of dissection method with Sluder guillotine.
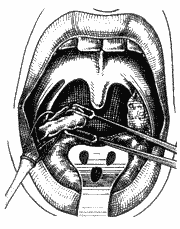
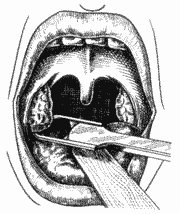
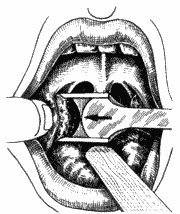
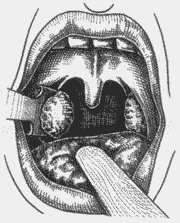
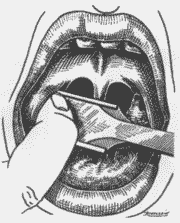
The patient was placed in a semi-seated position, forming a 45° angle from the horizontal plan, under general anesthesia with Halothane (halogen anesthetic) and orotracheal intubation; we placed Studer's mouth opener to expose the tonsils. We used anchored gauze on the hypopharynx to protect the lower airways. Next, we placed the inferior pole in the Studer guillotine (Figure 6), aided by the indicator finger of the opposite hand that pressed the anterior pillar (Figure 7), trying to protect the uvula and the muscles. Next, we pressed firmly the guillotine, making a clockwise upwards rotation movement on the right tonsil site (Figure 8) and anti-clockwise on the left tonsil site, to the lateral, resulting in medial, inferior and posterior vectors. At that point, after having dissected completely the tonsil, we used the indicator finger in hook (Figure 9) and maintained the pulled guillotine in order to extract the tonsils. Next, we proceeded with hemostasis using anchored gauze. If necessary, we used simple catgut 2-0 for suture.
Figure 8. Guillotine closure using clockwise rotation movements.
Figure 9. Dissection of tonsil with opposed indicator finger up to its extraction.
RESULTS
In order to analyze the results, we compiled data in tables.
Table 1 analyze§ the duration of surgery in minutes for both techniques. We observed, after using independent t test (p), that Sluder's technique takes significantly less time than the dissected technique (p<0.001). In Table 2, comparing blood loss in milliliters, there was no statistically significant difference between the techniques (p=0.229).
Table 3 shows the number of ligations demonstrating that in Sluder's technique the number of ligation was statistically significant lower than in the dissected technique (p=0.044).
As to debris of tonsil site (Table 4), we did not notice statistically significant differences between the surgical techniques using qui-square test, and the observed value was 0.00 and critical value was 3.84.
Table 5 analyzes the presence of fever on postoperative days 1, 7 and 14. We used qui-square test to analyze it. On the first post-operative day, the observed value was 1.92 and the critical value was 3.84; on days 7 and 14, the observed value was 0.00 and the critical value was 3.84. We concluded, therefore, that there were no statistically significant differences between the techniques concerning fever.TABLE 1 - Duration of surgery in minutes.
TABLE 2 - Blood loss in milliliter.
TABLE 3 - Number of ligations.
TABLE 4 - Tonsillar debris.
Key: N - number of cases.
TABLE 5 - Fever on post-op days 1, 7 and 14.
Key: N - Number of cases.
TABLE 6 - Bleeding on post-op days 1, 7 and 14.
We observed bleeding (Table 6) with both techniques on post-operative days 1, 7 and 14 and we did not detect statistically significant difference with qui-square test (observed value = 0.00; critical value = 3.84).
Table 7 demonstrates post-operative pain (post-op days 1, 7 and 14). When we applied the qui-square test, there was no statistically significant difference on day one (observed value = 0.05 and critical value = 5.99), on day seven (observed value = 1.30 and critical value = 3.84) or on day 14 (observed value = 0.00 and critical value = 3.84).
DISCUSSION
Reduction of morbidity in tonsillectomy benefits the patients, reducing hospital and drug costs1,3,7,11. Owing to a number of objections to the use of Sluder's technique, the procedure has lately become unpopular2,12, and therefore, there are no current medical residence programs that train young physicians on how to use Sluder tonsillectome. The reported disadvantages of the technique were lack of control of blood loss, remaining tonsil debris, accidents such as uvulectomy, partial accidental glossectomy and pillar damage, as well as blood aspiration into the lower respiratory trees10. However, some authors reported low incidence of post-operative bleeding and presented as one of the main advantages the speed of the procedure13, showing that appropriate application of the technique results in safe removal of tonsils, with no damage to other structures. The risk and unacceptable habit of using Sluder's guillotine without orotracheal intubation should not doom a good technique to failure, but it is in fact a dangerous technique depending on the kind of anesthesia used. Tonsillectomy with Sluder's technique may be considered a good option provided that it is appropriately employed, by experienced surgeons and under orotracheal intubation. If patients are intubated, well monitored and under appropriate care, all surgical procedures are safe, and Sluder's guillotine does bring advantages to the surgeon and the patient, as we concluded in the present study.
TABLE 7 - Pain on post-op days 1, 7 and 14.
(TABELA 7, PÁG. 324)
CONCLUSION
Based on the results, we concluded that:
- both procedures are equally good and efficient;
- tonsillectomy using Sluder's guillotine is statistically faster, requiring a smaller number of intra-operative ligations;
- analysis of morbidity was similar in both groups.
REFERENCES
1. CAPPER, J. W R.; RANDALL, C. - Postoperative Haemorrhage in tonsillectomy and Adenoidectomy in children., Laryngol. Otol., 98: 363-365, 1984.
2. CARMODY, D.; VAMADEVAN, T e COOPER, S. M. - Post-tonsillectomy Haemorrhage. J. Laryngol. Otol., 96: 363365, 1982.
3. CARITHERS, J. S.; GEBHART, D. E.; WILLIANS, J. A. Post-operative Risks of Pediatric Tonsilloadenoidectomy. Laryngoscope, 97: 422-429, 1987.
4. GLANTZ, S. A. - Primer of Biostatistics, 4ª ed., USA, Editora Mc.Graw Hill, 1997, 1-455.
5. HAASE, F. R. e NOGUERA, J. T. - Hemostasis in Tonsillectomy By Electrocautery Arch. Otolaryngol., 75: 125-126, 1962.
6. LEACH, J.; MANNING, S.; SCHAEFER, S. - Comparison of Two Methods of Tonsillectomy. Laryngoscope, 103: 619-622, 1993.
7. LINDEN, B. E.; GROSS, C. W; LONG, T E.; LAZAR, T H. - Morbidity in Pediatric Tonsillectomy. Laryngoscope, 100: 120-124, 1990.
8. MARTINEZ, S. A. e AKIN, D. E - Laser Tonsillectomy and Adenoidectomy. Otolaryngol. Clin. North Am., 20: 371376, 1987.
9: McAULIFFE, J. C. - The History of Tonsil and Adenoidal surgery. Otolaryngologic. Clinics of North America, 20: 415-419, 1987.
10. McGUIRE, N. - A Method of Guillotine Tonsillectomy With an Historical Review. Laryngoscope, 105: 187-194, 1995.
11. SALAM, M. A. a CABLE, H. R. - Post-tonsillectomy pain with diathermy and ligation techniques. A prospective randomized study in children and adults. Clin. Otolaryngol, 17- 517-519, 1992.
12. SIODLACK, M. Z.; GLEESON, M. J.; WENGRAF, C. L. Post-tonsillectomy secondary hemorrhage. Annals of the Royal College of Surgeons of England, 67: 167-168, 1985.
13. WAKE, M.; GLOSSOP, E - Guillotine and dissection Tonsillectomy compared. J. Laryngol. Otol, 103: 588-591, 1989.
14. WEIMERT, T. A.; BABYAK, J. W; RICHTER, H. J. Electrodissection Tonsillectomy. Arch Otolaryngol. Head and Neck Surg., 116. 186-188, 1990.
* Otorhinolaryngologist, Coordinator of the Advanced Course in Otorhinolaryngology at CLINORL - Institute, de Otorrinolaringologia a Oftalmologia, São Paulo/SP
** Resident Physician at CLINORL - Instituto de Otorrinolaringologia a Oftalmologia, São Paulo/SP
*** Otorhinolaryngologist at CLINORL - Instituto de Otorrinolaringologia a Oftalmologia, São Paulo/SP
**** Otorhinolaryngologist, Former Resident at CLINORL - Instituto de Otorrinolaringologia a Oftalmologia, São Paulo/SP
Study conducted at CLINORL - Instituto de Otorrinolaringologia a Oftalmologia, São Paulo /SP, and presented at the 34° Congresso Brasileiro de Otorrinolaringologia, on November 22, 1998, in Porto Alegre/RS.
Address correspondence to: Edson Carlos Miranda Monteiro - Av. Leôncio de Magalhães, 750 - 02042-000 São Paulo/SP - Tel: (55 11) 6950-2339.
E-mail: clin_orl@uol.com.br
Article submitted on June 26. 2000. Article accepted on January 18, 2001.