Year: 2013 Vol. 79 Ed. 6 - (23º)
Relato de Caso
Pages: 792 to 792
Low-power laser therapy in chemical-induced oral mucositis: a case study
Author(s): Niedson José de Siqueira Medeiros1; Nadson Frederico de Siqueira Medeiros2; Carla Caroline Medeiros dos Santos3; Georgia Veloso Ulisses Parente3; Januse Nogueira de Carvalho4
DOI: 10.5935/1808-8694.20130143
Keywords: drug therapy; laser therapy; oral medicine.
![]()
INTRODUCTION
Oral mucositis (OM) is a common complication of chemotherapy and (or) radiotherapy, representing respectively, 40% and 100 % of cases of oral mucosa inflammation1,2. Erythema, ulceration, bleeding, swelling and pain are among the symptoms and signs, compromising nutrition, speech and fluid intake of the patients, predisposing them to systemic infection3-5. The World Health Organization (WHO) classifies oral mucositis into: grade 0: absent; Grade 1: erythema, grade 2: erythematous and ulcerated, tolerating solids; Grade 3 : erythematous and ulcerated, tolerating liquids only; Grade 4: erythematous and ulcerated, precluding feeding3. The low power laser therapy (LPL) works in the prevention and treatment of OM, providing for analgesic and anti-inflammatory effects, greater patient comfort, maintaining mucosal integrity and better tissue repair2-6. With this paper we aim at analyzing the effectiveness of laser therapy in the treatment of oral mucositis.
CASE PRESENTATION
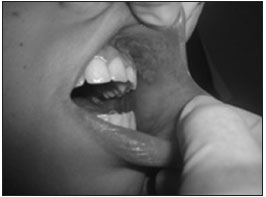
BMCR - department of pediatric oncology, a 15-year-old female diagnosed initially with Ewing's sarcoma in the right clavicle, submitted to chemotherapy with ifosfamide, etoposide and vincristine (doxorubicin in subsequent cycles) under parenteral nutrition, complaining of intense pain. She had febrile neutropenia and pancytopenia, the patient received packed red blood cells and platelets and granulokine, cefepime, fluconazole and nystatin. Undergoing orthodontic treatment, with poor oral hygiene, she developed grade 3 mucositis lesions (WHO) in the buccal mucosa and left retromalar triangle. The dentist removed the device, removed the biofilm and polished her teeth. Laser therapy was instated three times a week for treatment of the mucositis lesions. We started with the 780 nm wavelength (λ) and an energy density of 4.3 J/cm2, and analgesic agent around the lesions. In the second session, we employed the therapeutic LPL at λ 660 nm, at an energy density of 4.3 J/cm2, around the lesions (Figure 1). BMCR was instructed concerning oral hygiene and use of mouthwashes with chlorhexidine gluconate at 0.12%. After the first session, pain subsided and after the second, the patient was fed; after the fourth session, the lesions had decreased, healing almost entirely after the fifth application. A new cycle of chemotherapy was started two weeks later. Preventive laser at λ 660 nm, energy density of 1.3 J/cm2 per point in the region of the buccal mucosa, mouth floor, tongue and palate, three times a week, was applied in order to avoid lesion recurrence. Currently, in the fourth cycle of chemotherapy, the patient no longer developed mucositis lesions. Thus proving the functional and clinical efficacy of the LPL: accelerating wound healing, reducing pain and length of hospital stay.
Figure 1. Region submitted to the laser therapy (660 nm wavelength, energy density of 4.3 J/cm2) - buccal mucosa.
DISCUSSION
Oral mucositis is defined as an inflammation and ulceration of the oral mucosa with pseudomembrane formation and potential source of infection, particularly febrile neutropenia1, such as it happened with our patient (BMCR). Pathologically, in mucositis there is a shallow ulcer generating interstitial exudate, cellular debris and fibrin, producing a pseudomembrane analogous to a superficial skin scar. The chemotherapy-induced mucositis varies from 40 % to 76 % for patients treated with standard and high-dose chemotherapy, respectively1. In intensive chemotherapy for relapse after remission, the association with ifosfamide, carboplatin and etoposide, and irinotecan are known to be toxic for the oral mucosal2. Antimetabolite agents (methotrexate, cytarabine, mercaptopurine), alkylating agents (melphalan busulphan), antibiotics (Doxorubicin) and etoposide, both used by the patient, also induce mucositis1,2,6. In this case, the LPL eliminates pain already at the first application. This fact is attributed to the release of β-endorphin in the nerve endings of the ulcer, while promoting tissue biostimulation, quickly repairing the ulcerations2.
FINAL COMMENTS
It is necessary to encourage the use of low-power laser for the prevention and treatment of oral mucositis in cancer patients. It is a low cost and viable option in otorhinolaryngology, without side effects.
REFERENCES
1. Volpato LE, Silva TC, Oliveira TM, Sakai VT, Machado MA. Radiation therapy and chemotherapy-induced oral mucositis. Braz J Otorhinolaryngol. 2007;73(4):562-8. PMID: 17923929
2. Cruz LB. A influência do laser de baixa energia na prevenção de mucosite oral em crianças e adolescentes com câncer submetidos à quimioterapia [Dissertação]. Porto Alegre: Universidade Federal do Rio Grande do Sul; 2005.
3. Rampini MP, Ferreira EMS, Ferreira CG, Antunes HS. Utilização da terapia com laser de baixa potência para prevenção de mucosite oral: revisão de literatura. Rev Bras Cancerol. 2009;55(1):59-68.
4. Khouri VY, Stracieri ABPL, Rodrigues MC, Moraes DA, Pieroni F, Simões PB, et al. Uso do laser terapêutico para prevenção e tratamento da mucosite oral. Braz Dent J. 2009;20(3):215-20. DOI: http://dx.doi.org/10.1590/S0103-64402009000300008
5. Zanin T, Zanin F, Carvalhosa AA, Castro PHS, Pacheco MT, Zanin IC, et al. Use of 660-nm diode laser in the prevention and treatment of human oral mucositis induced by radiotherapy and chemotherapy. Photomed Laser Surg. 2010;28(2):2337. DOI: http://dx.doi.org/10.1089/pho.2008.2242
1. Medical Student, Federal University of Campina Grande, UFCG (Medical Student)
2. MD, Graduated from the Federal University of Paraíba, UFPB (Physician of the Family Health Program (Tavares, PB), Attending Physician - Regional Hospital José Pereira Lima (Princesa Isabel, PB))
3. Medical Student, Federal University of Campina Grande, UFCG (Medical Student)
4. Graduate in Dentistry, Pontifical Catholic University of Rio de Janeiro, PUC-RJ (DDS and dental expert and the Federal University of Campina Grande, UFCG)
Federal University of Campina Grande, UFCG.
Send correspondence to:
Niedson José de Siqueira Medeiros
Rua José Alves Medeiros. Bairro Cruzeiro
Princesa Isabel - PB. Brasil. CEP: 58755-000
Tel.: (0xx83) 9959-5550
Paper submitted to the BJORL-SGP (Publishing Management System - Brazilian Journal of Otorhinolaryngology) on August 1, 2012; and accepted on December 15, 2012. cod. 9741.
All rights reserved - 1933 /
2026
© - Associação Brasileira de Otorrinolaringologia e Cirurgia Cérvico Facial