Year: 2004 Vol. 70 Ed. 2 - (12º)
Artigo Original
Pages: 226 to 231
Acute diffuse external otitis: a prospective study in Rio de Janeiro's summer
Author(s):
Ricardo R. Figueiredo 1,
Magdala L. Fabri 2,
Walter S. Machado 3
Keywords: acute external otitis, predisposing factors, summer diseases
Abstract:
The acute external otitis is a very common disease in tropical countries, especially in summer. There are many predisposing factors and clinical features may vary, particularly the pain's severity. Aim: Evaluate, with a prospective study in Rio de Janeiro's largest Urgencies Hospital, the incidence and characteristics of the acute external otitis in summer. Study design: Clinical study with transversal cohort. Material and Method: 391 patients with acute external otitis in Souza Aguiar Hospital were evaluated in several clinical and treatment parameters, including predisposing factors analysis. Results: Pain, moderate ear discharge and sensation of "full ear" were the most common complaints. Sea and pool baths and the use of ear sticks were the most common predisposing factors. Conclusion: The acute external otitis is a very common disease in tropical countries, especially in summer. Sea and pools water contamination, although rejected by many authors as a predisposing factor, may have a role the patogenesis of the acute diffuse external otitis.
![]()
INTRODUCTION
Acute diffuse external otitis is an extremely common affection in tropical countries, amounting to a large number of emergency cases in Otorhinolaryngology, especially during summer 1, 2. It consists of acute and diffuse inflammation of the skin and subcutaneous cover of the external ear, predominantly caused by bacteria and whose main symptom is otalgia, which can be quite intense 1, 2, 3, 4, 5. Mucus-purulent otorrhea, generally in small amount, can also occur, as well as ear fullness sensation, hearing loss and pruritus 3, 4. The physical examination can show external auditory canal edema and hyperemia, with small amount of mucopurulent secretion 3, 4, 5. In some cases, the tympanic membrane may not be visible owing to marked edema in the external canal. In other cases, the tympanic membrane is thickened and hyperemic in its external cutaneous cover, which can give us the false impression that it is otitis media 6. Painful retro and pre-auricular adenomegalia can also be found, as well as edema of ear neighboring tissues.
Treatment is normally conducted with topical antibiotics, such as otological drops associated with local heat, symptomatic and non-steroidal antiinflammatory drugs (NSAID). Appropriate cleaning of epithelial debris and discharge made by the otorhinolaryngologist is also essential, being that systemic antibiotic therapy should be reserved for the most exuberant cases, with fever and evidence of complications, even though its use is attacked by many authors 1, 2, 3, 4, 5, 6, 7.
Our study intended to analyze the incidence of acute external otitis in the largest Emergency Hospital in Rio de Janeiro, Hospital Municipal Souza Aguiar, state reference for ENT emergency cases. Data were collected during the summer of 2002/03 and we recorded parameters according to predisposing factors, symptoms, physical examination and treatment.
MATERIAL AND METHOD
During the months of January to March 2003 we recorded data referring to 391 patients who had diagnosis of simple acute external otitis seen by the Service of Otorhinolaryngology and Perioral Endoscopy, Hospital Municipal Souza Aguiar, in Rio de Janeiro. The hospital is the state reference for ENT Emergency cases.
Patients were seen during day and night shifts, exclusively by the Otorhinolaryngologists authors of the present study.
The analyzed parameters were:
- gender
- age
- duration of symptoms
- otalgia, graded as mild, moderate and severe
- presence of otorrhea, pruritus, ear fullness and fever
- type of external otitis, according to our internal classification, as shown below
- presence of retroauricular adenomegalia and pre or retroauricular edema
- type of treatment
- predisposing factor
We used our own classification, according to the following criteria:
- TYPE 1 - only external auditory canal hyperemia
- TYPE 2 - external auditory canal edema, which does not prevent visualization of tympanic membrane and small amount of mucous-purulent discharge
- TYPE 3 - marked edema in the external auditory canal, preventing visualization of tympanic membrane.
Our classification used in this study aimed at assessing the severity of external otitis and guiding its treatment. Data were presented in descriptive form percentage.
RESULTS
As to gender, 45.92 % of the cases affected male and 54.08 % affected female subjects. As to age range, 10.20 % were aged 0 to 5 years; 7.14 % were 6 to 10 years; 23.47% were 11 to 20 years; 37.24 % were 21 to 40 years; 20.41 % were 41 to 60 years, and 1.54 % of the patients were over 60 years.
Out of the total, 33.16 % of the patients came to the hospital within the first 48 hours from onset of symptoms, 38.77 % between 48 and 96 hours, 19.90 % between 5 and 7 days and 8.17 % after 7 days from onset of symptoms.
There were 37.24 % of patients who reported mild otalgia, 47.45 % had moderate otalgia, and 15.31 % had severe otalgia. Mild otorrhea was reported in 29.08 % of the cases, pruritus in 20.41 %, low fever in 12.75 %, and ear fullness sensation in 46.43 % of the cases.
As to type of otitis, we observed 29.59 % type 1 cases, 48.47 % type 2 cases, and 21.94 % type 3 cases. Distribution by gender had a similar presentation than the general distribution, except for type 3, in which there was a clear prevalence of female gender (62.79% of the cases). As to duration of symptoms, we observed type 1 predominance in treatment provided within the first 48 hours (41.38%) of the cases, and types 2 and 3 between 48 and 96 hours (35.79 % and 46.51 %, respectively).
Pre- or retroauricular painful adenomegalia was found in only 8.67% of the cases, being that none of them had external otitis type 1. Similarly, periauricular edema was also found in only 8.67 % of the cases (out of the total, 5.88 % were type 1; 70.59 % were type 2; 23.53 % were type 3). A total of 15.61 % of the patients presented tympanic membrane with hyperemia, 90 % of them with grade 2 external otitis.
As to treatment, 89.29 % of the patients were treated only with prescription of drugs; 1.53 % with drug prescription and dressing, and 8.67 % with PO drug prescription and parenteral drugs, and 0.51 % with PO drug prescription, dressing and parenteral drugs. The latter, when used, comprised intramuscular analgesics (dypirone).
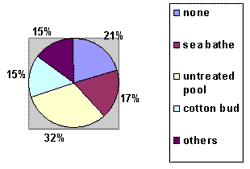
Upon analyzing the predisposing factors, we plotted the graph shown below.
There were other predisposing factors such as assault, showers or garden hose showers, swimming pool with chlorine, trauma caused by toothpick or hair clip, and river bathes.
DISCUSSION
Acute diffuse external otitis consists of acute infection of cutaneous and subcutaneous cover tissues of the external auditory canal from bacterial etiology 1, 2. The most frequently involved bacteria are Pseudomonas aeruginosa, Staphylococcus aureus, Escherichia coli, Proteus sp. and, more recently, anaerobe agents, such as Peptostreptococcus sp. and Bacteroides sp 8. According to some authors, some genotypes of Pseudomonas sp. can cause more severe external otitis than other types. 8
In our hospital, whose service of Otorhinolaryngology is exclusively directed to emergency services, external otitis is the most frequent ENT affection during summer, when it amounts to about 70% of the cases of Otorhinolaryngology. It is important to emphasize that during summer months, the Service of Otorhinolaryngology and Perioral Endoscopy at Hospital Souza Aguiar, can experience up to 50% increase in number of patients, which reinforces the importance of this affection during summer.
The most frequent predisposing factors were contact with water (which leads to skin maceration and removal of the protecting secretion of the external ear), use of cotton buds and other objects (toothpicks, hair clips, pen cap, etc), eczema and external auditory canal trauma 1, 2, 3, 5. On top of all these factors, in addition to trauma, there are changes in pH (alkalization), caused by increase in humidity and removal of cerumen (which is acid)2. Most of the studies tend to state that the contamination factors from water contact (sea, swimming pool) are irrelevant 5, 7. The contact with water favors maceration of skin of the canal and leads to removal of cerumen, which can lead to external otitis. However, some authors stated that Pseudomonas aeruginosa that cause external otitis can be part of the normal flora of the external auditory canal, and originate from other patients or even arise from different environmental sources 8. In our data, we observed high incidence of children who used to go swimming in untreated swimming pools, or in some specific beaches in Rio de Janeiro, which would theoretically favor the hypothesis of water contamination. However, such data should be carefully analyzed, since Hospital Souza Aguiar normally sees less privileged population groups of Rio de Janeiro, who frequently swim in untreated pools and specific beaches. We believe it is important to foster awareness about the use of swimming pools and the authorities should enforce seawater quality control policies. Future studies comparing bacteriological findings of seawater and those found in external otitis will be able to explain this issue.
Our incidence of predisposing factors is in agreement with the general literature, with predominance of sea/swimming pool bathes and use of traumatic objects in the ear, such as cotton buds 1, 2, 3, 4, 5, 6. The high incidence of external otitis after bathes in untreated swimming pools can be explained owing to the characteristics of the population seen by our service. As previously reported, the possible contamination of water should be carefully analyzed, but it should not be ruled out. For this reason, data on quality of beaches should also be carefully analyzed. We believe that in cases in which no predisposing factors are found, the probable cause is contact with shower water or deficient information provided by the patient.
Our data are in agreement with the literature concerning distribution by gender, without predominance (in our study, there were 54.08% female subjects) 2, 7. As to age distribution, the literature does not show preference to any age range 2, but our study showed higher incidence in the age range 21 to 40 years (37.24%), with lower incidence among elderly and children. However, we should carefully analyze the data since we believe that pediatricians see the highest percentage of pediatric external otitis cases. As to elderly patients, they probably go less frequently to swimming pools and beaches. There were no literature data concerning onset of symptoms and specialized treatment. In our study, 71.93% of the patients were seen within the first 96 hours. We would expect more patients seen within the first 48 hours (which was only 33.16%) considering that it is a painful pathology, but the deficiency of ENT services in Rio de Janeiro, allied to the preference for use of natural treatments, family recommendations and otological medications provided over-the-counter, and fear to be absent from work, among others, can seem to explain the figures.
Most of the patients referred moderate otalgia (47.45%). The most frequent symptoms according to the literature were otalgia (present in all reports), mild mucous-purulent otorrhea (29.08% of our patients), otological pruritus (20.41%), and ear fullness (46.43%) 1, 2, 3, 4, 5, 6, 7. Fever was not a common symptom, which is in agreement with the literature (12.75%). The distribution of cases with fever concerning gender, age range and type of otitis were similar to the general distribution.
Data referring to type of external otitis, in which we followed our own classification, strongly suggested that the three types comprised the many different stages of disease progression. External otitis starts with mild otalgia and hyperemia of the external auditory canal (type 1), followed within 48 to 96 hours by worsening of otalgia, mild otorrhea, ear fullness and sometimes otological pruritus and fever. Otoscopy normally shows edema on the external auditory canal, still allowing visualization of the tympanic membrane, with small amounts of thick mucus-purulent discharge (type 2). In some cases, especially in the absence of appropriate treatment, or owing to agent's virulence (bacteria), it progresses to marked edema of the external auditory canal, completely occluding the lumen and preventing visualization of the tympanic membrane (type 3). It is important to point out that we should be extra careful in managing external otitis in diabetic patients owing to the possibility of malignant external otitis.
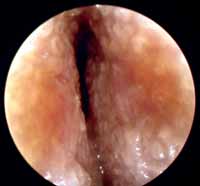
We did not find data in the literature about satellite adenomegalia and edema of the neighboring areas and hyperemia of the tympanic membrane, which proved to be not very frequent findings (8.67% and 8.67%, respectively). Hyperemia of the tympanic membrane was found in 15.61% of the cases, being that 90% of them in external otitis type 2. In type 3 cases, the same would probably have occurred but, in most cases, the tympanic membrane was not visible owing to marked edema of the external auditory canal (Figure 3). Tympanic membrane hyperemia is one of the main factors that question the differential diagnosis of external otitis and otitis media, but absence of tympanic perforation in the presence of external otitis speaks in favor of the latter. The correlation of clinical presentation is obviously extremely important for differential diagnosis of both affections. However, even for highly experienced otorhinolaryngologists, there may be some questionable cases, which should be treated with preventive antibiotic therapy, especially if considering the social-economic conditions of the patients and the poor status of public healthcare system in Brazil.
As to treatment, most of the patients (89.29%) were treated only with prescription of drugs. In our routine, based on the experience of the center, we follow the criteria below:
- type 1 - otological drops + general guidance
- type 2 - NSAID + otological drops + general guidance
- type 3 - systemic corticoids (in the absence of contraindication) + systemic antibiotics (cefalexine, cefadroxil or quinolones) + general guidance.
Varied otological drops are available in the market. Most of them consist of the association of corticoids, anesthetics, neomycin and polymyxin B. Neomycin is effective against S. aureus and Proteus sp. Polymyxin B is effective against the same germs and also against Pseudomonas aeruginosa. Many patients develop allergic reactions to neomycin. Quinolones, such as ciprofloxacyn are effective against all referred germs, but according to some authors, there is a tendency of quick development of resistance against them 9. There are still chloramphenicol drops, efficient against gram-negative anaerobe agents 1, 9, 10.
The best option for systemic antibiotics is quinolones, efficient against S. aureus and P. aeruginosa 9,10. However, they are expensive drugs and rarely available in the public healthcare setting, leaving room for first generation cephalosporins, effective against S. aureus. Quinolones are contraindicated in children owing to the risk of inhibition of bone growth. The option for use of antibiotics and systemic corticoids in cases of external otitis type 3 reflects the experience of our center, but there are some authors that discourage the use of this type of treatment compared to topical treatment.
The general guidance provided includes dry local heat, otological protectors (including cotton balls soaked in oiled substances) and no use of cotton buds and other traumatic objects. Dressings should be made in cases of abundant discharge in order to facilitate topical treatment. We can also make use of symptomatic drugs via parenteral administration. We are against the use of multiple gauze dressings on the external auditory canal as recommended by many authors for topical treatment 5, 7, since it is a very painful procedure that provides almost no advantage compared to conventional treatment. Since there is no controlled study about the method, we would like to emphasize that this is only the personal opinion of the authors.
As a result of our treatment routine, the incidence of visits to the hospital because of lack of symptom improvement amounts to only 6%. Even though one can argue that patients that do not improve end up looking for a different center, we do not believe this is a relevant issue considering the poor social economic conditions and the poor status of the healthcare system in Rio de Janeiro, leaving very few other options to patients. Therefore, we believe that this percentage (6%) is representative of our rate of therapeutic failure.
Some studies recommended the use of drugs in powder, associating dexamethasone, oxytetracycline, polymyxin B and nistatin, since powder would help reduce the humidity of the external auditory canal 10. However, we have no experience in its use.
CONCLUSION
External otitis is a very common disease in tropical countries, being that sea and swimming pool bathes and use of cotton buds and other sharp instruments into the ear are among the main predisposing factors. Water contamination, despite being ruled out by many as a predisposing factor, can play a role in the pathogenesis, but the confirmation of this hypothesis depends on the conduction of future bacteriological studies. The different clinical-otoscopic aspects probably represent different stages of the progression of the disease, which responds well in most of the cases to clinical treatment, especially under the form of NSAID, symptomatic and otological drops.
ACKNOWLEDGEMENT
To all Otorhinolaryngologists and LPNs working at Hospital Municipal Souza Aguiar.
Graph 1- Predisposing Factors.
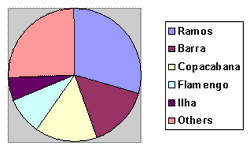
Graph 2- Distribution of beaches.
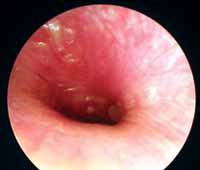
Figure 1- Acute Diffuse External Otitis Grade 1.
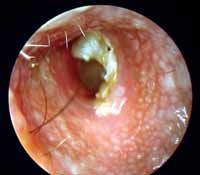
Figure 2- Acute Diffuse External Otitis Grade 2.
Figure 3- Acute Diffuse External Otitis Grade 3.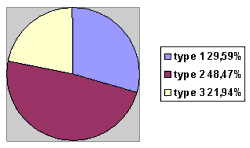
Figure 4- Classification of external otitis.
REFERENCES
1-Daneshrad, BA; Jenny C. Kim, MD; Amedee, R.G.: "Acute Otitis Externa", J La state Med Soc, 2002; vol 154: 226-7..
2-Diniz Júnior, J.: "Otite Externa", Revista Brasileira de Medicina, ORL, 1997; vol. 4, nº 4:106-11.
3- Saffer,M. et al. "Otite Externa Difusa Aguda", Revista AMRIGS.1983; 27:194-6
4-Hungria, H.: "Otorrinolaringologia", 7ª Edição, Rio de Janeiro,Editora Guanabara -Koogan,1995:307
5-Bremond, G.;Wayoff,M.; Chobaut,J.C.; Magarna,J.; Aquaviva,F.: "Pathologie de l'oreille externe", Encyclopedie Médico-Chirurgale, Paris, France, Oto-rhyno-laryngologie, 1980; 200070 A,9:3-7.
6-Kyrmse, R.J.: "Noções de ORL Pediátrica",2 ª Edição, Fundo Editorial BYK-Procienx, 1976:29-36.
7-Balkany,T.J.;Bradford, D.R.: "Infections of the external ear", in Cummings CW (ed):Cummings Otolaryngology Head and Neck Surgery. MO, Mosby, 1997, 2979-986.
8-Matar,GM; Harakeh,HS; Ramwali,F; Khneisser,I; Hadi,U.: "Comparative analysis between Pseudomonas aeruginosa genotypes and severity of symptoms in patients with unilateral or bilateral otitis externa", Current Microbiology, Vol. 42, 2001: 190-3.
9-Arnes,E;Dibb,WL:"Otitis externa: clinical comparison of local ciprofloxacyn versus local oxytetracycline, polymyxin B, hydrocortisone combination treatment", Current Med Res Opin 13, 1993:182-6.
10-Goldenberg,D; Golsz,A; Netzer,A; Joachins,HZ: "The use of otic powder in the treatment of acute external otitis", American Journal of Otolaryngology, vol 23, n º 3, 2002:142-7.
1 Otorhinolaryngologist, Hospital Municipal Souza Aguiar, Rio de Janeiro.
2 Otorhinolaryngologist, Hospital Municipal Souza Aguiar, Rio de Janeiro.
3 Head of the Service of Otorhinolaryngology and Perioral Endoscopy, Hospital Municipal Souza Aguiar, Rio de Janeiro.
Study conducted at Hospital Municipal Souza Aguiar, Rio de Janeiro
Address correspondence to: Ricardo R. Figueiredo, Rua 60, n 1680, apt 202, Sessenta, Volta Redonda-RJ, CEP 27261-130, fax (55 24) 3349-8664, e-mail otosul@uol.com.br.