Year: 2004 Vol. 70 Ed. 2 - (2º)
Artigo Original
Pages: 156 to 162
Microsurgery in nasal poliposis: clinical and surgical evolutive analysis
Author(s):
Denise Abritta 1,
Alexandre Rafaldini Coraçari 2,
José Victor Maniglia 3
Keywords: nasal poliposis, microsurgery, risk analysis
Abstract:
Aim: The present study purpose was to investigate the nasal polyposis endonasal microsurgery efficacy, evaluating the number of disease recurrence according to sex, age, stage and patients' professions examined at the Otholaryngology Department and Head and Neck Surgery, Medical School, São José do Rio Preto-FAMERP. Study design: Clinical study with cohort longitudinal. Material and method: Thirty patients were submitted to endonasal microscopic surgery in the period of 1991 to 1996, 16 females and 14 males in a post-operative follow-up from one to five years. Results: Recurrence frequency was 40 %, and the predominance was statistically significant (chi-square and Fisher tests, values p=0.03 and 0.024, respectively) in males (75%). Synechia complication could be observed in four (13,3 %) cases. Conclusion: It was concluded that endonasal microsurgery in nasal polyposis has permitted 60 % of the patients to be free from recurrence of disease in the follow-up period, with greater frequency among males. This technique showed to be effective in the nasal polyposis treatment, just presenting synechia complication in 13.3 % of the cases.
![]()
INTRODUCTION
Nasal polyps are prolapse of the upper respiratory mucosa such as edema of stroma, which can be classified as nasosinusal pseudotumors 1. Hippocrates (460-370 BC) had already described the many different types of nasal polyps and methods to remove them, but the disease remains up to present as a significant clinical problem, especially because of the high incidence of recurrence.
Etiology is still obscure and it seems that persistent local inflammation is essential for the development of nasal polyps, which may occur in diseases such as Woakes' syndrome, cystic fibrosis, congenital mucociliary disease or Kartagener's disease, aspirin intolerance, among others 2-4.
Recent studies have shown that the nasal mucosa cavity (meatus region, concha or septum) is the site of origin for the polyp, whose most frequent site is the ostium of ethmoid cells 5. Antronasal polyps originate from the maxillary sinus and are more common in children and young adults 5.
The symptoms of nasal polyposis are in general characterized by progressive nasal obstruction, which may be complete depending on disease staging, rhinorrhea that is predominantly serous, headache and olfaction disorders. In the physical examination, there is the possibility of widening of the nasal pyramid basis in more advanced cases. Anterior rhinoscopy can show formations of edematous aspect, pale gray color, with large water content and poor vascularization.
Endoscopy is very useful for diagnosis and postoperative follow-up, especially in small polyps of the middle meatus. Radiology is important to determine anatomical variations 7 and the level of sinus commitment, allowing staging of polyposis and differential diagnosis with neoplastic processes 8. Simple x-ray incidences are mentalis-nasal and frontal-nasal-plaque and for computed tomography, there are axial and coronal sections.
As to clinical treatment of polyposis, antibiotic therapy and topical and systemic corticoids have been widely used. Preoperatively, this management allows reduction of inflammatory and infectious processes, allowing surgical maneuvers especially by reducing bleeding 9, 10.
Environmental control is very important as a prophylactic therapeutic support, as well as specific hyposensitizing immunotherapy 11, 12, and the use of sodium chromoglycate 13.
In the progression of the surgical treatment of the nasal polyps, the polypotome created by Fallopius and Fabricius in the 16th century was the first instrument used to remove them. Katakura (1794) in Japan and Sigong (1617) in China were the first ones to record the removal of polyps in their respective countries. In the 19th century, cauterization and caustic techniques, as well as the use of cold loop, adrenaline and cocaine became common 14.
George Caldwell (Nova York, 1893), Scanes Spicer (London, 1894) and Henri Luc (Paris, 1897) described transbuccal radical maxillorhinostomy as the modern surgery to solve the problem of maxilla anthritis. The operation technique by Caldwell-Luc consists of access through the canine fossa to the maxillary antrum and opening of the nasoantral window below the inferior nasal concha 15. It was considered the main approach to the maxillary sinus for the treatment of chronic maxillary sinusitis and removal of lesions such as polyps. Ethmoidectomy was also conducted through this access 16.
Montgomery & Wilson, in 1982, described intranasal ethmoidectomy without the support of microscopy in cases of repetitive obstructive nasal polyposis, using as a reference the insertion of the medium concha to locate the ethmoid cells. In very extensive polyposis, they indicated external ethmoidectomy 17.
Endonasal microsurgery consists of the use of surgical microscope and special instruments to treat nasosinusal diseases, using the access through the nasal cavity. Heermann (1958) was the first to employ the microscope in the transnasal surgery. Authors such as Messerklinger, Golding Wood, Prades, Dixon, Wigand, Draf, Kennedy, Stammberger and others were responsible for adding new knowledge about the techniques and the use of special instruments to perform nasosinusal surgeries 18.
Many authors in the past 25 years have indicated the use of microscope in the surgical treatment of nasal diseases 13, 18-20. The evolution of endonasal microsurgery has occurred thanks to mastery of the anatomical knowledge of the nasosinusal region 21, 22. Owing to its complex anatomy, this region is surrounded by structures such as the orbit, skull base and vital vascular-nervous elements, such as internal carotid, cavernous sinus and cranial nerves. Therefore, it is essential to be precise in surgical procedures in the area, preventing complications.
Complications can be classified into major and minor severity levels. The minor ones, represented by synechia, crusts, ecchymosis, palpebral edema, among others, are followed by low morbidity and do not compromise patients' life. Major complications, such as optical nerve lesion, cerebrospinal fluid fistula, internal carotid artery damage, cavernous sinus and others, present significant morbidity, with the possibility of death 23.
In addition to direct trauma of the intraorbital structures in the region, there is the risk of vascular spasms, caused by injection of anesthetics and corticoids in the nasal mucosa, which can lead to postoperative amaurosis after nasosinusal surgeries 24.
The purpose of the present study was to assess the efficacy of endonasal microsurgery to treat nasal polyposis, considering the complications and number of recurrence episodes of the disease according to gender, age, staging and jobs of the patients seen in the Department of Otorhinolaryngology and Head and Neck Surgery, Medical School, Sao José do Rio Preto, SP - FAMERP.
MATERIAL AND METHOD
We assessed 30 patients with diagnosis of nasal polyposis and indication of surgical treatment, be it by advanced disease or clinical non-tractability, referred to endonasal microsurgery by the Department of Otorhinolaryngology and Head and Neck Surgery, Medical School, Sao José do Rio Preto - FAMERP, in the period between 1991 and 1996. We excluded from the study patients that had underlying diseases (arterial hypertension, diabetes, cardiopathy, lung pathology, etc) and did not present optimal clinical conditions to be submitted to surgical procedures with general anesthesia.
The age of patients ranged from 12 to 70 years, mean age of 34 2.9 years, being that in this study we considered three age ranges: 10 to 30 years, 31 to 50 years, and 51 to 70 years. Among them, 16 (53%) were female and 14 (46.7%) were male. Most of the patients - 22 (73.3%) had nasal polyposis stage IV, 7 (23.3%) had stage III and 1 (3.3%) had stage V. As to jobs, 10 patients were housewives, 5 were students, 4 were rural workers, 3 were mason workers. The others were tinsmith, welder, mechanical engineer, polisher, carpenter, storage assistant, sale clerk and office clerk.
The staging used to classify the level of invasion of polyposis was based on the classification modified by Stamm (1995), being that:
- Stage I: Middle concha, middle meatus
- Stage II: Anterior ethmoid -maxillary sinus
- Stage III: Stage II / Nasal cavity +1 Sinus
- Stage IV: Paranasal sinuses / Nasal cavity
- Stage V: Extra-sinusal extension
Complications were classified into major and minor. Major complications were divided as: 1. Orbital: blindness, orbital hematoma and diplopia; 2. Intracranial: CSF leak, meningitis, pneumoencephalus; cerebral abscess, intradural hematoma, cavernous sinus thrombophlebitis; cranial nerve damage; and 3. Hemorrhage.
Minor complications were divided into: 1. orbital: edema, ecchymosis, subcutaneous emphysema, and nasolachrymal duct damage; 2. Facial pain (infraorbital nerve lesion); 3. Mild hemorrhage; 4. Crusts; and 5. Synechia.
All patients were submitted to preoperative investigation, including clinical assessment and Otorhinolaryngological examination with rhinoscopy, conducted with rigid endoscope (0o or 30o and 4mm) or flexible nasolaryngoscope, if necessary. They were also submitted to paranasal sinuses CT scan at axial and coronal sections, whose results indicated location and staging of polyposis.
The patients were submitted to endonasal microsurgery for removal of nasal polyposis. Surgeries were conducted under general anesthesia with orotracheal intubation and controlled arterial hypotension, if necessary, and if the general status of the patient allowed it.
The patient was placed on the surgical bed in supine position, elevating the head region from the horizontal plan to reduce venous bleeding. The surgeon was seated contralaterally to the operated side. Before the surgery began and during the procedure drops of topical vasoconstrictors were used in the nasal cavity with cold saline solution to control bleeding.
Surgical microscope with objective lenses of 250mm and straight ocular lenses with special instruments were also used. Polyps were removed from the middle meatus, where pedicles are normally positioned. The middle concha was luxated towards the nasal septum, where the autostatic speculum was placed, being preserved and maintained under constant visualization during the conduction of ethmoidectomy via endonasal approach. Ethmoidectomy was initiated, in most of the cases, by removing the ethmoidal bulla. Next, the other ethmoidal cells were removed from anterior-posterior direction up to sphenoid, proportional to the extension of the disease, preserving as much mucosa as possible.
To access the maxillary sinus, the unciform process and other structures of the middle meatus were removed using blunt end instruments and angulated curettes. During the surgical act, the head position of the patient and the surgical microscope were moved according to the approached paranasal sinuses.
Once the surgery was concluded, a plastic mold made with the plastic from the saline solution vial (normally 250ml, since it was thinner), was placed over the nasal septum bilaterally, fixed with mononylon 4-0 thread, which remained in place for 7 to 10 days, in order to prevent formation of synechiae.
Outpatient postoperative follow-up was made with rigid endoscope (0o, 30o and 4mm) or flexible nasolaryngoscope. The interval between the surgery and follow-up was one to 5 years, considering in the assessment aspects such as recurrence, gender, age range, staging, complications and jobs classified as of higher or lower risk of recurrence.
As to statistical analysis, we used Fishers' tests to compare frequency of recurrence between male and female patients after endonasal surgery to remove nasal polyposis. The chi-square test was used in the comparative tests of frequency of recurrence between male and female genders, age range, different stages of the disease, and patients' jobs. We adopted the significance for p value below 0.05.
RESULTS
The results obtained in the study of 30 patients submitted to endonasal microsurgery to remove nasal polyposis are presented considering the number of recurrences according to gender, age, staging and patients' jobs. Table 1 presents 18 patients (60%) that had no recurrence in 1 to 5 years follow-up.
The number of recurrences by gender is shown in Table 2, which reveals statistically significant higher incidence of recurrence in male (75%) than in female patients (25%) (chi-square and Fisher's test, values of p=0.03 and 0.024, respectively).
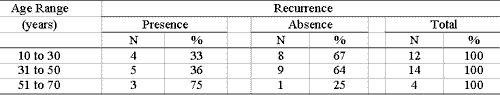
The study of patients by age range showed higher frequency and increased recurrence as age increased. Table 3 shows the presence of nasal polyposis recurrence in three (75%) out of 4 patients aged 51 to 70 years, whereas in the age range of 10 to 30 years, it occurred in four (33%) out of 12 studied patients. However, there was no statistically significant difference between age range and presence or not of recurrence (chi-square test, value p=0.31).
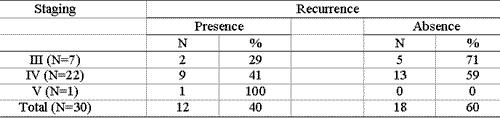
The frequency of recurrence by staging of nasal polyposis is shown in Table 4. There was a trend in evolution of level of invasion of polyposis and occurrence of recurrences, since 9 (41%) out of the 13 patients in stage IV presented disease recurrence. Moreover, the only patient in stage V also presented recurrence, whereas 5 (71%) of the seven patients in stage III were free from recurrence in 1 to 5-year follow-up. However, there was no statistically significant difference between staging and presence or absence of recurrence (chi-square test, value of p=0.39).
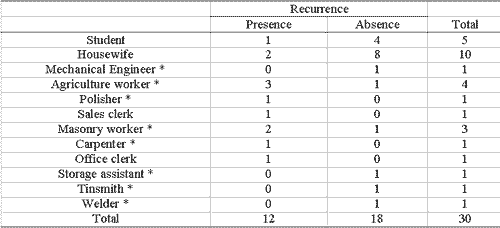
Table 5 shows the frequency of recurrence according to jobs. It is noticed that three (75%) out of four patients with rural jobs had recurrence, which also happened with 2 (67%) of three masonry workers with nasal polyposis.
There were no major complications in this study. As to minor ones, there were only synechiae in 4 patients (13.3%).
DISCUSSION
Endonasal microsurgery conducted in 30 studied patients proved to be definitive in controlling nasal polyposis in 60% of the patients with 1 to 5-year follow-up. In this case, 12 patients (40%) presented recurrence in which 10 were treated with clinical management and two were reoperated since they had significant obstructions. The results are in agreement with those reported by Teatini et al. (1991)25, whose surgical procedure was also anterior-posterior middle meatus dissections in most cases. They presented occurrence of 40% of recurrence after endonasal microsurgery in 78 patients with polyposis, which were followed up for at least 2 years, and they detected complications in 15 cases (19.2%) with orbital ecchymosis. Thanks to combined used of microscope and endoscope to treat polyposis in 22 patients with minimum follow-up of 1 year, the authors found recurrence of 23% (5 cases), and as complications there were three cases (13.7%) of orbital ecchymosis. The frequency of complications reduced, and owing to case evolution, they reported lower incidence of recurrence in the treatment of maxillary sinus polyps, which is facilitated by the use of angulated endoscope.
Conversely, reduced recurrence was detected by Wigand & Hosemann (1989) in a study with 600 patients submitted to microendoscopic endonasal ethmoidectomy to treat polyposis 26. Postoperative endoscopic control showed recurrence of polyps in 18% (30 cases), mucosa hyperplasia in 25% (42) and mucosa thickness in 5% (8) of them. The mucosa was normal in 52% of the patients. They used different types of techniques according to staging of polyposis. The technique of retrograde ethmoidectomy described by Wigand in 1981 26 was conducted for severe diffuse polyposis of the whole ethmoid and other sinuses, visualized by preoperative computed tomography.
However, these authors presented higher number of complications, such as fistula (0.3%), owing to rupture of olfaction tract, which was detected and immediately closed with mucosa and fibrin glue. There was loss of olfaction in 3% of the cases, obstruction of lachrymal duct in 0.5% and postoperative meningitis in 0.5% of them. There were no cases of visual disorders.
Bagatella & Mazzoni (1986) published 110 cases (71%) of olfaction loss or reduction in 155 cases (100% of patients submitted to endonasal ethmoidectomy with microscope) 13. Intraoperative complications occurred in six cases (4%), with rupture of meninges and CSF leak. These cases were immediately treated with lyophilized dura graft and fibrin glue. As late complications, there were synechia in 13 cases (33%) of the 40 first operated cases and they were treated by removing the synechia and using silastic for two weeks. The authors used an operative technique that removed completely the middle nasal concha to better expose the middle and upper meatus, which could explain the complications that occurred.
In this study there were no orbital, intracranial or hemorrhagic complications. We detected four (13.3%) cases that progressed with synechia without related complaints. We also observed significantly higher frequency of recurrence in male subjects (75%). However, there are no literature reports about it. In the analysis of patients' jobs, we highlighted the jobs exposed to allergens and toxic agents. It seems to reinforce the action of other factors involved in the etiopathogenesis of the disease, which should be investigated in future studies.
In the analysis of 60 patients with nasal polyposis, Schumacker & Randall (1996) observed that onset of nasal obstruction and diagnosis of the disease took less than 2 years27. They concluded that polypoid nasal disease was an entity with short evolution in most patients, being that long histories and/or investigations were not frequent. It is applicable due to technology advances of CT scan and endoscopic tests 28.
In this study, we detected that the more advanced the grade of nasosinusal polyposis, the smaller the number of recurrences, indicating the importance of early diagnosis. In these cases, we used the endoscope as a support for diagnostic and postoperative control. The instrument was very useful, since it presented possibility of angulations. Currently, endoscopic nasal surgery has been employed in our service (Department of Otorhinolaryngology and Head and Neck Surgery, FAMERP) as the preferred method to treat nasosinusal polyposis, being the use of microscope an option, according to the preference and familiarity of the surgeon.
Fang (1994) studied 71 patients aged 10 to 62 years with chronic sinusitis and nasal polyposis who were submitted to functional endoscopic surgery 29. They conducted a preoperative analysis of clinical history, skin allergic tests, assessment of mucociliary function and endoscopic test. The abnormalities found by the endoscope on the maxillary antrum mucosa were divided by the authors into three groups: thickness, edema and polyposis. All patients were examined one week after the surgery and from then on, they were regularly treated with suction and irrigation of maxillary antrum. The disease was considered persistent in cases in which the mucosa did not recover after 17 weeks.
The author highlighted the presence of edema (87%), causing recovery of 96% of the cases before 16 weeks and only 31% for the group of polyposis that presented persistent disease up to the 17th week. There was no statistically significant difference concerning persistence of disease in allergic and non-allergic groups, however recovery of antral mucosa was longer with persistence of disease in the group with compromised mucociliary function. It was concluded that preoperative assessment of the clinical history, allergic and mucociliary function, as well as endoscopic exam, could serve as reference to control time of recovery and modality of treatment.
In our study, outpatient postoperative control was made within 7 to 10 days after removal of the mold, which prevented synechia, and after the interval of two to three weeks depending on the need to remove crusts and clean the nasal cavity in each case.
The 30 patients of the study were submitted to preoperative CT scan at axial and coronal sections to document disease staging and the occurrence of anatomical variations. The importance of preoperative CT scan assessment for the surgeon to locate the disease and define its extension was highlighted by Bolger et al. (1991), who analyzed 202 CT scans for endoscopic surgeries at coronal incidence and detected anatomical variations of paranasal sinuses bones in 64.9% of the patients, including pneumatization and paradoxical curve of the middle concha, Haller's cells and pneumatization of uncinate process 7. Mucosa abnormalities were detected in 83.2% of the patients.
Weber et al. (1992) analyzed double-plan high resolution CT scan for preoperative diagnosis of 158 patients aged between 8 and 81 years, with chronic rhinosinusitis and nasal polyps 30. They detected that in chronic sinusitis and nasal polyposis, the anterior ethmoid was the most frequently involved sinus followed by maxillary, frontal, posterior ethmoid and sphenoid sinuses. The high number of anatomical variations of the middle meatus could justify the excessive occurrence of anterior ethmoid infections. Other variations were detected, such as presence of optical nerve in the lateral region of the posterior ethmoid, named Onodi's cells, and dehiscence of the bone wall of the internal carotid, and optical nerve in the sphenoid sinus. High resolution CT scan allowed visualization of paranasal sinusal complex and its relation with vital neighboring structures.
Endonasal microsurgery provides safety to the surgical process, owing to better visualization of anatomical structures, facilitating the control of bleeding and the removal of polyps, which reduces the rate of recurrence. The procedure is not very traumatic, reducing the risk of complications. The use of microscope presents as advantages binocular stereoscopic vision, different grades of magnification, bimanual work, excellent lighting, and the possibility of photographic documentation and filming, contributing to medical education. As to disadvantages, it allows only unidirectional view without angulations, in addition to requiring trained surgeons.
CONCLUSION
The use of endonasal microsurgery to manage nasal polyposis resulted in 60% of patients free from recurrence in a 1 to 5-year follow-up.
Male subjects were more frequently affected by recurrence than female subjects.
Postoperative complications were scarce in patients submitted to surgical treatment of nasal polyposis, and we observed only synechia, which demonstrated that endonasal microsurgery is a safe surgical procedure when performed by experienced hands.Table 1. Number of patients according to presence or absence of recurrence after endonasal microsurgery in a five-year follow-up.
Table 2. Number of male and female patients considering presence or absence of recurrence after endonasal microsurgery.
Table 3. Number of patients considering presence or absence of recurrence after endonasal microsurgery according to age range.
Table 4. Number of patients considering presence or absence of recurrence after endonasal microsurgery according to staging.
N = number of patients
Table 5. Number of patients considering presence or absence of recurrence after endonasal microsurgery according to jobs.
* Jobs with higher risk of exposure to allergens and toxic agents.
REFERENCES
1. Stamm AC & Watashi CH & Pozzobon M. Microcirurgia dos Tumores Benignos Naso-Sinusais. In: Stamm AC. Microcirurgia Naso-Sinusal. Rio de Janeiro: Editora Revinter Ltda; 1995. p. 343-6.
2. Mygind N. Pólipos nasais. "Bolsas cheias de líquido" In: Alergia. Um Texto Ilustrado. Rio de Janeiro: Editora Revinter; 1993. p. 324-8.
3. Stávale JN. Histopatologia Naso-Sinusal. In: Stamm AC. Microcirurgia Naso-Sinusal. Rio de Janeiro: Editora Revinter Ltda; 1995. p. 140.
4. Augusto AGLBS, Granato L, Santos GG, Carvalho MFP. Síndrome de Woakes: A Propósito de Dois Casos. Rev Bras de Otorrinolaringologia 1998; 64(1): 81-6.
5. Larsen PL & Tos M. Origin of nasal polyps. Laryngoscope 1991; 101: 305-12.
6. Gomes CC, Sakano E, Chung HM, Melo RRG. Origem e conduta nos pólipos antrocoanais. Rev Bras de Otorrinolaringologia 1992; 58 (1): 10-20.
7. Bolger WE, Butzin CA, Parsons DS. Paranasal Sinus Bony Anatomic Variations and Mucosal Abnormalities: CT Analysis for Endoscopic Sinus Surgery. Laryngoscope 1991; 101: 56-64.
8. Abritta D & Padovani Jr JA. Estudo de caso em otorrinolaringologia. Enlace 1991; 39: 25 e 30.
9. Camp VC & Clement PAR. Results of oral steroid treatment in nasal polyposis Rhinology 1994; 32: 5-9.
10. Kanai N, Denburg J, Jordana M, Dolovich J. Nasal Polyp Inflammation: Effect of Topical Nasal Steroid American Journal of Respiratory and critical care medicine 1994; 150: 1094-100.
11. Cavalcanti PF. Bases Imunológicas da Alergia Naso-sinusal. In: Stamm AC. Microcirurgia Naso-Sinusal. Rio de Janeiro: Editora Revinter Ltda; 1995. p. 126-8.
12. Dixon HS. Microscopic sinus surgery transnasal ethmoidectomy and sphenoidectomy Laryngoscope 1983; 93: 440-4.
13. Bagatella F, Mazzoni A. Microsurgery in Nasal Polyposis Transnasal Ethmoidectomy. Acta Oto Laryngologica 1986; 431: 1-19.
14. Pahor AL, Kimura A. History of Removal nasal polyps. F Med 1991; (BR)102 (5): 183-6.
15. Ünlü HH, Çaylan R, Nalça Y, Akyar S. An Endoscopic and Tomographic Evaluation of Patients with Sinusitis after Endoscopic Sinus Surgery and Caldwell-Luc Operation: A Comparative Study. The Journal of Otolaryngology 1994; 23 (3): 197-203.
16. Tobin HA. Cirurgia de Los Maxilares. In: Paparella MM, Shumrick DA. Otorrinolaringologia. Cabeça y Cuello. Buenos Aires: Editorial Médica Panamericana 1982; 3: 2697.
17. Montgomery WW, Wilson WR. Cirurgia de Los Senos Frontales Etmoidales y Esfenoidales In: Paparella MM, Shumrick DA. Otorrinolaringologia. Cabeça y Cuello. Buenos Aires: Editorial Médica Panamericana 1982; 3: 2102-7.
18. Stamm AC. (a) Cirurgia Microendoscópica Naso-Sinusal. In: Microcirurgia Naso-Sinusal. Rio de Janeiro: Editora Revinter Ltda; 1995.p. 183-213.
19. Bosch J. Microcirurgia Coanal. In: Prades J, Bosch J, Tolosa A. Microcirurgia Endonasal. Madrid: Gráficas Orbe S.L; 1977. p.267.
20. Faugère JM, Fleyss J, Aubert C, Nottet JB, Gonteyron JF. Sinusites chroniques: indications et résultats du traitements par microchirurgie endonasale. Revue Laryngol 1988; 109 (2): 113-9.
21. Mcminn RMH, Hutchings RT, Logan BM. A cavidade nasal. O hiato maxilar e o canal nasolacrimal In: Atlas Colorido da Cabeça e do Pescoço. Netherlands: Livraria Editora Artes Médicas Ltda.; 1991. p.62.
22. Navarro JAC. Anatomia dos Seios Paranasais e Estruturas Correlatas. In: Stamm AC. Microcirurgia Naso-Sinusal. Rio de Janeiro: Editora Revinter Ltda; 1995.p. 15-36.
23. Stamm AC. (b) Complicações da Microcirurgia Naso-Sinusal. In: Microcirurgia Naso-Sinusal. Rio de Janeiro: Editora Revinter Ltda; 1995.p. 255-63.
24. Siebert DR. A Amaurose como Complicação de Cirurgias Naso-Sinusais. Rev Bras de Otorrinolaringologia 1995; 61 (1): 64-9.
25. Teatini GP, Stomeo F, Bozzo C. Transnasal Sinusectomy with combined microscopic and endoscopic technique. The Journal of Laryngology and Otology 1991; 105: 635-7.
26. Wigand ME, Hosemann W. Microsurgical treatment of recurrent nasal polyposis Rhinology 1989; 8: 25-30.
27. Schumacher DV, Randall CJ. A survey to determine the extent of previous symptoms and surgery on patients presenting with nasal polyps. The Journal of Laryngology and Otology 1996; 110: 736-8.
28. Lourenço EA. Sinusites. Da abordagem diagnóstica à orientação terapêutica. RBMORL 1997; 4 (3): 70-82.
29. Fang SY. Normalization of maxillary sinus mucosa after Functional endoscopic sinus surgery (FESS). A prospective study of chronic sinusitis with nasal polyps. Rhinology 1994; 32: 137-40.
30. Weber A, May A, Ilberg C, Halbsguth A. The value of high resolution CT-Scan for diagnosis of infectious paranasal sinuses disease and endonasal surgery. Rhinology 1992; 30: 113-20.
1 Master in Otorhinolaryngology and faculty member, Medical School, Sao José do Rio Preto (FAMERP).
2 Resident physician, Department of Otorhinolaryngology and Head and Neck Surgery, FAMERP.
3 Full Professor, Head of the Discipline of Otorhinolaryngology and Head and Neck Surgery, FAMERP and General Director of FAMERP.
Study conducted at the Department of Otorhinolaryngology and Head and Neck Surgery, Medical School, Sao José do Rio Preto - FAMERP - SP.
Study submitted as Master Dissertation, Medical School, Sao José do Rio Preto, in 1999.
Address correspondence to: Denise Abritta - Travessa das Camélias nº 45 Jd. Seixas 15061-140 Sao José do Rio Preto - SP.
Tel (55 17) 232-3977 E-mail: deniseabritta@yahoo.com.br