Year: 2003 Vol. 69 Ed. 1 - (4º)
Artigo Original
Pages: 24 to 27
Head and neck rhabdomyosarcoma in childhood
Author(s):
Beatrice Mª J. Neves, 1;
Paulo A. de L. Pontes, 2;
Eliana M. Caran, 3;
Claudia Figueiredo, 4;
Luc L.M. Weckx, 5;
Reginaldo R. Fujita 6
Keywords: rhabdomyosarcoma, pediatric oncology, head and neck neoplasm
Abstract:
Rhabdomyosarcoma (RMS) is a malignant tumor of immature mesenchymal cells; it can arise from any part of the body. RMS is the most common soft tissue sarcomain the childhood and its most frequent primary site is the head and neck.
AIM: The purpose of this study was to review the occurrence of head and neck RMS in childhood and its clinical-histopathologic features.
STUDY DESIGN: Clinical retrospective.
METHOD: Eighty-two patients with soft tissue sarcoma treated in the Institute of Pediatric Oncology, UNIFESP-EPM, between 1988 and 2002 were included in this study. The medical records of the patients with head and neck soft tissue sarcomas were reviewed. The following parameters were analyzed: incidence of RMS in the childhood and in the head and neck, sex, age, histological classification, primary site, follow-up.
RESULTS: In this study, 65% of soft tissue sarcomas were RMS; 33% of RMS were in the head and neck region; 77% of soft tissue sarcoma in this region were RMS. The mean age at diagnosis was 7.62 years, 41% were between 5 and 9 years. In this sample, there were 47% men and 53% women. Embryonic RMS was the predominant histological type (64.6%) and the orbit was the most common primary site (52.8%). One hundred percent, 50% and 33.3% of the parameningeal, nonparameningeal and orbital RMS, respectively, led to death.
CONCLUSION: RMS is the most common soft tissue sarcoma in the childhood and the head and neck is the most frequent primary site. Males were more affected by RMS than females. The mean age at diagnosis was 7.62 years and the most frequent age interval was between 5 and 9 years old. The embryonic histological type and the orbit as primary site were predominant. The highest mortality was found for parameningeal RMS and the lowest, for orbital RMS.
![]()
INTRODUTION
Rhabdomyosarcoma (RMS) is a malignant neoplasia originated from primitive mesenchymal cells. It is a soft tissue sarcoma that is frequent in children, may affect any body part and the clinical expression of the disease is directly related to its location. The most frequent primary site of RMS is the head and neck, followed by the genital-urinary tract and the extremities1, 2, 3. Considering all sarcomas of head and neck soft tissues, RMS is also the most common4, 5. It has predominance in male patients with two peaks of incidence: in the first decade of life and in the second one.
There are various histopathologic classifications for RMS. The one adopted by our service is the International Classification of Rhabdomybsarcoma. This classification includes the following subtypes: botryoid, spindle cells, embryonal, alveolar, undifferentiated and without other specifications 6. The most frequent histology type is embryonal. Botryoid RMS is considered a subtype of embryonal RMS; it has the most favorable prognosis1, 2, 3, 7, 8.
Intergroup Rhabdomyosarcoma Study (IRS) is a multidisciplinary, multicentric team comprising researchers from large training centers in cancer in the US and Europe. IRS has conducted various protocols that studied biology and treatment of RMS in children since 1972, and the results have guided the management of RMS cases in various countries.
The first IRS (IRS-1) classified patients with RMS in 4 clinical groups based on extension of disease and type of surgery conducted (table 1).9-10
The survival was related to the clinical group that the patient belonged. A study performed by the IRS showed that the 5-year survival rate for patients in clinical groups I, II, III, IV was 83%, 70%, 52% and 20%, respectively.1Table 1. IRS - Clinical Groups.
For the head and neck, the IRS defined three large anatomical regions of primary affection by RMS that were significant for the prognosis orbital, parameningeal, nonparameningeal. The parameningeal location is the most frequent one and involves: infratemporal fossa, nasopharynx, middle ear, mastoid and paranasal sinuses. Nonparameningeal location included all the other areas: parotid, submandibular region, scalp, oropharynx, larynx1, 2, 10. Orbital RMS is the one that has the best prognosis. The next best prognosis was of nonparameningeal RMS and lastly, the parameningeal, since it is difficult to perform complete surgical resection of the lesions in this location. IRS I referred 5-year survival rates of .89%, 55% and 47% for orbital, nonparameningeal and parameningeal lesions, respectively1.
In addition to type of histology, location of lesion and resectability, prognosis depends on size of tumor and vascularization. Larger and more vascularized tumors have worse prognosis.
The treatment of choice for RMS is combination of surgery, chemotherapy and radiotherapy as demonstrated in the studies by IRS1, 2, 7. In addition to these studies, the main, form of treatment for RMS is surgery, with poor survival rates. &tow et al. analyzed retrospectively medical charts of 78 children with diagnosis of RMS treated in the period between 1946 and 1966, observing a 5-year overall survival of 28%11. With combined therapy, 5-year overall survival increased to 55% in IRS I and 63% in IRS II1, 2.
The purpose of the present study was to analyze the, occurrence of head and neck RMS in children and the respective clinical-histopathologic and evolution aspects.
MATERIAL AND METHOD
Eighty-two patients with diagnosis of sarcoma of soft tissue seen by the Institute of Pediatric Oncology, Federal University of Sao Paulo - Escola Paulista de Medicina (UNIFESP - EPM) in the period between August 1998 and April 2002 were included in the present study. We selected 24 medical charts of patients with head and neck affections (lesions located above the plan formed by the clavicle and the body of the 7th cervical vertebra). We excluded two incomplete medical charts. Of the analyzed charts, we collected the following data: gender, age, histologic classification, clinical group, location of lesion and evolution. In our sample, no patient was submitted to surgery as definite therapy, and the surgical procedure was limited to biopsy. Histology classification was made by the Department of Clinical Pathology, UNIFESP-EPM. Patients were classified retrospectively according to the clinical groups determined by IRS.
We studied the following parameters:
1. Incidence of RMS in childhood;
2. Incidence of head and neck RMS in childhood;
a) Distribution by gender;
b) Distribution by age range;
c) Distribution by histology;
d) Distribution by primary location;
e) Death x lesion location;
f) Cause of death.
RESULTS
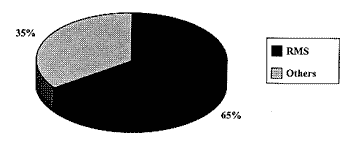
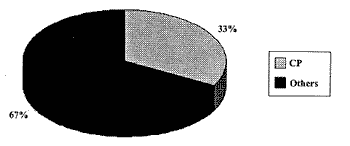
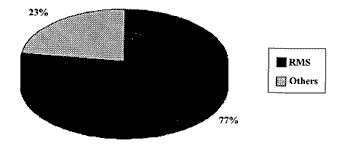
Out of the total of soft tissue sarcomas that were included in the study, 52 cases corresponded to RMS (Graph 1), being that 17 cases were located in the head and neck (Graph 2). We found 22 cases of soft tissue head and neck sarcomas, from which 17 were RMS (Graph 3). The five remaining cases of soft tissue head and neck tumor were: orbital alveolar sarcoma, mandible leiomyosauoma, maxillary sinus fibrosarcoma, mandible fibrosarcoma, lip mesenchymal neoplasm.
As to the 17 patients with diagnosis of head and neck RMS, the findings were:
o Age of patients ranged from 4 months to 20 years, mean age of 7.62 years.
o Eighty-eight percent of the patients belonged to the clinical group III and 12% to the clinical group IV.
Graph 1. Percentage of RMS (n=52) compared to other soft tissue sarcomas in childhood (n=28)
Graph 2. Percentage of RMS located on the head and neck - CP (n=17) compared to other locations (n=35)
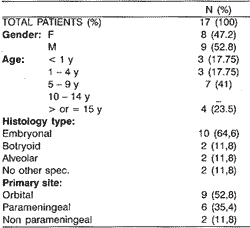
o Table 2 shows a descriptive analysis of the data found.
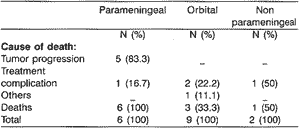
o Table 3 shows a percentage of death relative to location of tumor, analyzing the cause of death.
DISCUSSION
In our study, 33% of the case of RMS were located in the head and neck region. The Intergroup Rhabdomyosarcoma Study I (IRS I) followed 686 patients up to 21 years of age, with diagnosis of RMS for a period of 7 years; they observed an incidence of RMS in this region of 37%1. Similarly to the first study, IRS II followed up 999 children and found an incidence of 34% of head and neck RMS2. Karakas et al conducted a retrospective study of medical charts of 51 patients and the incidence of head and neck RMS was 31.4%3.
Graph 3. Percentage of RMS (n=17) compared to other soft tissue head and neck sarcomas (n=5)
Table 2. Descriptive Analysis
Table 3. Death / Cause of death X Tumor location
RMS is a soft tissue sarcoma more common in the head and neck and in children. In the present study, RMS was responsible for 77% of the neoplasia in the region. Weber et al., upon the analysis of medical charts of 188 adolescent and adult patients with soft tissue sarcoma of the head and neck also found a large number of cases of RMS in this region, but the incidence was much lower (18%)4. In adults, there are other soft tissue sarcomas to be considered, which are important owing to its greater incidence, such as for example, liposarcoma, hystiocytoma, angiosarcoma and leiomyosarcoma.
As to primary site of affection, we found about 53% of the patients with orbital compromise. The literature points to the parameningeal location as the most frequent one, 50% of the case of head and neck RMS are in this location10.
The most frequent histology type in this study was embryonal RMS (64.6%), followed by botryoid (11.8%)4. IRS I and II classified RMS using the Conventional System: alveolar, embryonal, botryoid, pleomorphic and undifferentiated RMS. In the study conducted by IRS I and II, respectively, 56% and 51% of the cases were embryonal RMS1, 2. Karakas et al. also observed predominance of this histologic type in 80.4%3.
Eighty-eight percent of the patients were in the clinical group III, 12% in group IV. The literature also shows a higher prevalence of clinical group III. According to Karakas et at., the percentages for patients in clinical groups I, II, III, IV were 3.9%, 23.6%, 47%, 25.5%, respectively.3 As to clinical group, IRS I found the following results 15%, 25%, 41%, 19%, belonging to groups I, II, III, IV, respectively1. Similarly, IRS II showed the following proportions 12.5%, 17%, 53.25%, 17, 25% in groups I to IV, respectively2. In this population, this study did not show patients in groups I and II. It is due to the fact that no patient could be submitted to surgery as definite therapy, owing to the lesion location,. The surgical procedure was limited to biopsy.
The mean age at diagnosis was 7.62 years, with predominance of the age range of 5 to 9 years (41%). IRS I observed mean age of 7 years, with predominance of age range 1 to 4 years (34%)1. Karakas et at. and Daya et al. reported mean age of 4.5 and 4.9 years, respectively3, 7.
The literature points to the predominance of head and neck RMS in male subjects (59%)7. In our study, we found 53% of male patients.
Of the 7 alive patients, 5 were free from the disease, all with diagnosis of embryonal RMS (1 botryoid), of orbital location, belonging to the clinical group III. Of the 2 alive patients with the disease, one presented parotid alveolar RMS, belonging to group IV, resistant to treatment, and the other had recurrent orbital RMS.
One hundred percent of the patients with RMS in parameningeal location died, most of them by tumor progression, confirming the worst prognosis of the lesion in this location.
CONCLUSION
Based on the study of the 80 cases of head and neck soft tissue sarcoma in children we concluded that rhabdomyosarcoma:
1. Is the soft tissue sarcoma more common in children as a whole, as well as in the head and neck;
2. There were differences concerning gender distribution, with male gender predominance;
3. It was more common in the age range 5 to 9 years;
4. The most common histology type was embryonal;
5. In the head and neck, the orbit was the most frequent primary site;
6. Parameningeal RMS presented the highest rate of death, especially as a result of tumor progression. Orbital RMS presented the lowest rate, usually caused by treatment complication.
REFERENCES
1. Maurer HM, Beltangady M, Gehan EA et al. The Intergroup Rhabdomyosarcoma Study-I: a final report. Cancer 1988; 61:109-220
2. Maurer HM, Gehan EA, Beltangady M et al. The Intergroup Rhabdomyosarcoma Study II. Cancer 1993; 71:1904-1922.
3. Karakas Z, Agaoglu L, Biner B et al. Results of Rhabdomyosarcoma treatment in a developing country. Acta Med Okayama 2000; 54(4):173-177.
4. Weber RS, Benjamin RS, Peters LJ et al. Soft Tissue Sarcomas of the Head and Neck in Adolescents and Adults. Am J Surg 1986; 152:386-392.
5. Gorsky M, Epstein JB. Head and Neck and intra-oral soft tissue sarcomas. Oral Oncology 1998;34:292-296.
6. Asmar L, Gehan EA, Newton WA, et al. Agreement among and within Groups of Pathologists in the Classification of Rhabdomyosarcoma and Related Childhood Sarcomas. Cancer 1994; 74:2579-2588.
7. Daya H, Chan HSL, Sirkin W Forte V. Pediatric Rhabdomyosarcoma of the Head and Neck. Is There a Place for Surgical Management? Arch Otolaryngol Head and Neck Surg 2000;126:468-472.
8. Wharam MD, Beltangady MS, Heyn RM et al. Pediatric Orofacia and Laryngopharyngeal Rhabdomyosarcoma. An Intergroup Rhabdomyosarcoma Study Report. Arch Otolaryngol Head and Neck Surg 1987;113:1225-1227.
9. Maurer HM, Moon T, Donaldson M et al. The Intergroul Rhabdomyosarcoma. A Preliminary Report. Cancer 1977;40:2012 2026.
10. Wexler LH, Helman LJ. In: Pizzo PA, Poplack DG. Principles and Practice of Pediatric Oncology. 3ª edição. Philadelphia: Lippincot Raven Publishers; 1997. 799
11. Sutow WW, Sullivan MP, Ried HL et al. Prognosis in Childhood Rhabdomyosarcoma. Cancer 1970;25:1384-1390.
1 Post-graduate studies under course, Department of Otorhinolaryngology and Human Communication Disorders, Federal University of São Paulo- Escola Paulista de Medicina.
2 Faculty Professor, Department of Otorhinolaryngology and Human Communication Disorders, Federal University of São Paulo - Escola Paulista de Medicina.
3 Assistant Professor, Institute of Pediatric Oncology, Federal University of São Paulo -Escola Paulista de Medicina.
4 Post-graduate studies under course, Department of Otorhinolaryngology and Human Communication Disorders, Federal University of São Paulo - Escola Paulista de Medicina.
5 Associated Professor, Department of Otorhinolaryngology and Human Communication Disorders, Federal University of São Paulo - Escola Paulista de Medicina.
6 Head of the Clinic, Discipline of Pediatric Otorhinolaryngology, Department of Otorhinolaryngology and Human Communication Disorders, Federal University of São Paulo - Escola Paulista de Medicina.
Affiliation: Study conducted at the Discipline of Pediatric Otorhinolaryngology, Department of Otorhinolaryngology and Human Communication Disorders, Federal University of São Paulo - Escola Paulista de Medicina.; presented at the 36° Congresso Brasileiro de Otorrinolaringologia, on November 19 - 23, 2002.
Address correspondence to: Dra. Beatriçe Mª J. Neves. Rua dos Otonis, n° 684, V. Clementino, São Paulo-SP, CEP: 04025-001. Tel/ fax: (55 11) 5539-7723. E-mail: asabranca@uol.com.br.
Article submitted on December 04, 2002. Article accepted on January 23, 2003.,