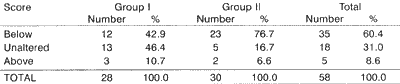Year: 2001 Vol. 67 Ed. 3 - (8º)
Artigos Originais
Pages: 346 to 354
Acute Lesions in the Larinx by Prolongated Tracheal Intubation and the Influence of the Tracheostomy in their Evolution.
Author(s):
Manos S. Coelho*,
Wilson S. Stori Jr.**.
Keywords: intubation, tracheostomy, lesion, larynx, flexible bronchoscopy
Abstract:
Material and Aim: This study analyses prospectively 73 patients in the ICU of the Hospital Cajuru (PUC-PR). The aim was to analyse the lesions in the larynx by the prolongated trasnlaryngeal tracheal intubation. Study design: Clinical prospective. Method: Fibrolaryngotracheobronchoscopy was performed on the 61th, 14th, 21st, 282th, 60th, 90th and on the 180th days. Results: The incidence of the hyperemia was detected in all patients; edema, in 45 (61,6%); and ulcer, in 51 (69,9%). The score of lesions varied from six to 23, with an average of 14,7. We studied the evolution of the lesions, the time of resolution of the laryngeal injury (TRLI), and the influence of the tracheostomy in their evolution in the 30 survivers. Conclusion: The TRLI lasted 28 days in 14 patients (46,7%); between 29 and 60 days, in 10 patients (33,3%); between 61 and 90 days, in two patients (6,7%); between 91 and 180 days in two patients (6,7%). In 53 patients (91,4%) the lesions either improved or remained unchanged, and in five of them (8,6%) the lesions aggravated after tracheostomy.
![]()
INTRODUCTION
The definition of prolonged tracheal intubation (PTT) is an unanimous concept and it applies both for intubation for more than 8 hours6,2 and for really prolonged intubation, as observed by Via-Reque and Rattemborg17, who published six cases of patients intubated for 55 to 155 days. Lindholm13, in his study, considered prolonged intubation if it exceeded 24 hours. Lindholm13, in a prospective study, found a 63% rate of acute laryngeal lesions in patients submitted to PTI, which were reversible in 30 days. The author observed 0.5 % of laryngeal stenosis in adults, and 6.7% in children, being that 80% of the adults and 33% of the children had been intubated for fewer than 36 hours.
Stauffer et al.15, in a prospective study with 150 patients with tracheal intubation and tracheotomy, found 95% of laryngeal damage at autopsy and 7.4% of long term subglottic stenosis.
Colice et al.15, in their series of patients, found 94% of acute laryngeal lesions; however, only 3 % required tracheotomy because of laryngeal damage.
The present study aimed at studying laryngeal lesions on the 6th day of PTI, its evolution, predisposing, triggering or aggravating factors, and its relation with early tracheotomy in patients admitted to the General ICU of Hospital Universitário Cajuru, Pontifícia Universidade Católica do Paraná.
MATERIAL AND METHOD
We prospectively studied 73 patients submitted to PTI in the General ICU of Hospital Universitário Cajuru, Pontifícia Universidade Católica do Paraná, from August 1, 1994 to July 31, 1995.
There were 63 male (86.3%) and 10 female (13.7%) patients - aged from 16 to 92 years. The mean age was 36.0 years.
Inclusion criteria in the study
Patients submitted to PTI for five consecutive days, who seemed to require it for seven days more; patients with no orotracheal intubation in the same hospitalization; patients with no previous laryngeal damage; patients with no laryngeal trauma; patients submitted to tracheotomy on the 6th day after PTI.
We required informed consent from patients or family members to perform clinical and endoscopic control on days 6, 14, 21, 28, 60, 90 and 180.
Patients were intubated with endotracheal silicone PVC tube (Willy Rusch AG)®, number 7.5 or 8 to women, and 8 or 8.5 to men, using oral approach. They were fixed with strings and knots around the tube and neck, using upper incisors as repair.
Tracheotomies were conducted on the sixth day of TI by surgeons of the Service of General Surgery or the Service of Thoracic Surgery, under supervision and technique standardization conducted by the author of the present study. Tracheotomy was performed in two different ways:
a) longitudinal incision of second and third tracheal rings (35 patients);
b) resection of a segment on the anterior wall of the second or third tracheal rings (38 patients).
We used fiberbronchoscope Olympus BF IT10, coupled to a light source Storz Xenon-615, with adapter Storz 495-D. Photographic documentation was performed with camera Olympus OM 10 and adapter Olympus A10 (M1 0.8x), and Kodak Ektakrome 160 ASA Tungsten film.
We used nasal approach in 71 patients. If nasal approach was unavailable or contraindicated because of anatomical conditions, hemorrhage or craniofacial trauma, we used oral approach, applying a protective mouth piece among the incisors (two patients).
Fibrolaryngotracheobronchoscopy (FLTB) were conducted under topic nasal anesthesia in the nostrils, nasal fossa, pharynx and glottic and supraglottic portions of larynx, with Xylocaine 1% spray; for subglottic larynx, trachea and bronchi we used Xylocaine liquid 1% by puncture through the cricothyroid membrane. In patients with tracheotomy cannula, we used 5ml of Xylocaine 1 % by transcricoid approach, and 5ml directly through the tracheotomy cannula, in order to anesthetize the subglottic region and the trachea, respectively.
We used a classification described by Lindholm13, Whited18 and Benjamin1 to quantify acute laryngeal lesions (Chart 1).
Total score was determined by the sum of acute lesion scores found in epiglottis, right arytenoid, left arytenoid, interarytenoid region or posterior commissure, right vocal fold, left vocal fold, and subglottic region. Vocal folds were analyzed and classified based on its anatomic and functional integrity.
Seventy-three patients were studied in order to determine incidence of laryngeal lesions caused by PTI, initial classification (mild, moderate, severe), evolution, correlation with variables age, gender, analysis of coma level by Glasgow score (below or above 7), neuromuscular activity (yes, no), previous hypotension (yes, no), bronchial aspiration (yes, no), presence of nasogastric tube (yes, no), infections during intubation (yes, no), and type of lesion or disorder.
Arterial hypotension was defined as systolic BP below 90mmHg for more than one hour.
Tracheobronchopulmonary infections were defined in patient who had clinical manifestation of tracheobronchopulmonary secretion, positive culture on pulmonary lavage, pulmonary condensations attributed to pneumonic and bronchopneumonic processes or pulmonary suppurations, and association with fever and/ or leukocytosis or different associations of the symptoms.CHART 1 - Classification of acute laryngeal lesions by PTI.
We identified and classified lesions on the 6th day using FLTB, and defined the correlation between the lesion and the variables listed above.
After the assessment of initial lesions, patients were divided into two groups: Group I (patients with tracheotomy who died during hospitalization), and Group II (survival patients). We compared the evolution of laryngeal lesions after tracheotomy between the two groups. In group II patients, we studied in details the evolution of laryngeal lesions, plus healing time and resolution time of laryngeal damage. We observed the times on days 28, from 29 to 60, from 61 to 90, from 91 to 180 and after day 180.
We used Student's t parametric test and chi-square and Mann-Whitney parametric tests in order to perform all the necessary comparisons. All applied tests were for independent samples. Minimal significance level was 0.05.
RESULTS
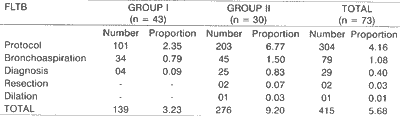
We conducted 415 FLTB in 73 patients and for the purpose of the present study we considered the evaluations on days 6, 14, 21, 28, 60, 90 and 180, amounting to 304 FLTB (Table 1).
Types of laryngeal acute lesion on 6th day after PTI
Hyperemia was detected in all patients. Edema was found in 45 patients (61.6%), divided by severity as follows: 36 (49.3%) were mild, 6 (8.2%) were moderate and 3 (4.1%) were severe, leading to glottic obstruction. Ulcers were found in 51 (69.9%) of the patients: in 11 patients (15.1%), it was mild, in 39 (53.4%), moderate and in one case (1.41%), severe. In addition, there was one patient with glottic circular ulcer, with exposure of cartilage.
The main location of ulcers was the glottis (44 cases, 86.3%), but there were three cases (5.9%) of association with epiglottic ulcer and two cases (3.9%) of association with subglottic ulcer. In two patients (3.9%) lesions were located only in the epiglottis
Initial score
The initial score of laryngeal lesions on day 6 of PTI varied from 6 to 23, mean of 14.7 ± 3.6.
Classification of laryngeal lesions on the 6th day of PTI (initial class)
Mild initial class was found in 25 (34.2%) of the patients; moderate class in 44 (60.3%), and severe in 4 (5.5%) cases. Among the latter, three of them were classified as severe because they had severe edema and one patient had ulcer and exposure of cartilage.
Resolution time of laryngeal damage in group II patients
In 14 (46.7%) of the patients, resolution time was 28 days, and there was no statistically significant difference among patients with or without ulcer.
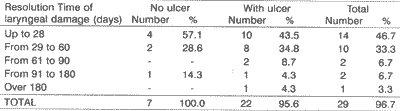
In 10 (33.3%) cases, resolution time was between 29 and 60 days and there was no statistically significant difference concerning presence or not of ulcer; in two cases (6.7%) resolution time was between 61 and 90 days, in two (6.7%) it was between 91 and 180 days, and in one case (3.3%) there was no resolution after 180 days (Table 2).TABLE 1 - FLTB in patients submitted to TTI followed by tracheotomy.
NOTE: The calculation of proportion was based on the total number of patients in each group.
TABLE 2 - Resolution time of laryngeal damage concerning ulcer in group II.
NOTE: One patient was not evaluated for resolution time because he had a translaryngeal mold.
One patient was not evaluated on 180th day because he had laryngeal mold as a complement of laryngoplasty for glottic and subglottic stenosis.
Presence or absence of ulcer and resolution of lesions up to the 20 day did not produce statistically significant difference.
Length of hospital stay varied from 14 to 170 days and there was statistically significant difference (p=0.0026) compared with resolution time.
The permanence of tracheotomy varied from 11 to 175 days when compared to resolution time, showing statistically significant difference (p=0.0052).
The duration of mechanical ventilation varied from 2 to 35 days and there was no statistically significant difference concerning healing time of laryngeal damage.
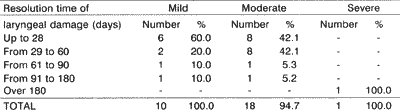
As to initial class, out of 10 patients with mild initial class, 6 of them (60%) had damage healed within 28 days, whereas in the group with initial moderate class comprising 18 patients, only 8 (42.1%) had the lesions healed within the same period. On the 60th day, eight patients (80%) of the mild initial class and 16 (84.2%) of the moderate class had their lesions healed (Table 3).
Evolution of laryngeal lesions caused by PTI after tracheotomy in groups I and II
In 35 (60.4%) out of 58 patients from both groups submitted to a second FLTB, there was improvement of scores of laryngeal damage after tracheotomy; in 18 cases (31.0%), the lesions remained unaltered and in 5 cases (8.6%), there was worsening of lesions (three patients from group I and two from group II) when compared to the first FLTB (Table 4).
There were 53 (91.4%) patients who showed improvement or no alterations of lesions after tracheotomy, but there was no statistically significant difference comparing groups I and II.
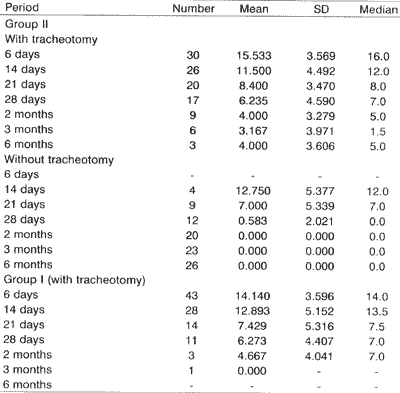
Evolution of laryngeal lesions, evaluated through the score of lesions of patients submitted to transtracheal intubation followed by tracheotomy on the 6th day, showed improvement of lesions, but there was no statistically significant difference among patients in group II - with tracheotomy, and patients in group I, decreasing the median score from 16 to 7 and from 14 to 7, respectively, on day 28 (Table 5). From then on, the mean score of group I was stabilized up to patients' death, and in group II the score decreased but did not reach the mean score of zero.TABLE 3 - Resolution time of laryngeal damage concerning initial class in group II.
NOTE: One patient was not evaluated for resolution time because he had a translaryngeal mold.
TABLE 4 - Variation of score of laryngeal lesions after tracheotomy in patients submitted to a second FLTB.
SOURCE: Chart A1A, from Annex 1, and Chart A2B from Annex 2
FLTB = Fibrolaryngotracheobronchoscopy.
In Table 5, we observed that the mean score of group II patients with and without tracheotomy decreased similarly. However, as from the 2151 day, the reduction of scores in patients whose tracheotomy had been removed became more marked, and in these patients lesions were completely cured after 60 days. The mean score of patients with tracheotomy on day 90th was three, and in six months, there was a slight increase to four. Three patients remained with the cannula after day 180, with median score of 4.
In group II patients, removal of tracheotomy produced statistically significant difference concerning laryngeal damage healing, as opposed to patients who maintained the tracheotomy.
Complications
Ten patients (13.6%) had complications from PTI four cases (5.5%) of selective intubation, one case (1.3%) of barotrauma pneumothorax; two cases (2.7%) of accidental extubation; two cases (2.7%) of difficulty/ impossibility to occlude the airways with the cuff; one case (1.3%) of necrosis in the 2nd - 61 tracheal rings, observed at tracheotomy, leading to death.
There were 15 (20.1%) occurrences of tracheotomy complications: three cases (4.1%) of stoma erosion; 4 (5.5%) of stoma infection; one case (1.3%) of subcutaneous emphysema; one case (1.3%) of slight hemorrhage from cervical vessels; two cases (2.7%) of stoma lateralization because of vicious head and neck position; three cases (4.1%) of accidental decannulations, with no further consequences, two of them in the same psychopathic patient; one case (1.1%) of tracheal stenosis between the cricoid and the stoma, attributed to compression of tracheal anterior wall by the tracheotomy cannula.
Two of the patients (2.7%) had tracheal stenosis on the junction of middle and inferior thirds, which may be attributed to compression caused by the cuff of the endotracheal tube of the tracheotomy cannula, that is to say, caused by tracheal intubation and/or tracheotomy.
DISCUSSION
Laryngeal lesions by PTI: initial classification
Whited18, in a prospective study of 200 patients submitted to FLTB to observe laryngeal lesion caused by PTI, using Lindholm13 classification, found laryngeal and tracheal mucosa alterations after extubation in 100% of the cases. However, the author did not present details about the initial findings.TABLE 5 - Comparative analysis of patients' scores with and without tracheotomy in group II and all patients in group I.
SOURCE: Chart A1A - Chart A2B. (1) Too high standard deviation. It is recommended to use median values.
Colicel found laryngeal lesions caused by PTI in 77 (94%) of 82 patients, classified as 34 (41.5%) mild lesions, 24 (29.2%) moderate lesions, and 19 (23.1%) severe lesions, using a classification similar to Lindholm's and the one used in the present study.
Lindholm13, in a series of 161 patients submitted to PTI for variable periods of time, described 35 cases (22%) with lesions grade I, 93 (58%) with lesions grade II, 29 (18%) with lesions grade III, and 4 (2%) with lesions grade IV.
Thomas et al.16, in 150 patients submitted to tracheal intubation for more than 24 hours, found laryngeal lesions in the initial assessment in 134 (87.6%) of them.
In the 73 patients assessed by the present study, we observed laryngeal damage in all of them, divided into 25 (34.2%) mild cases, 44 (60.3%) moderate cases, and four (5.5%) severe cases.
The differences among various series of laryngeal damage in the literature may be due to differences in the studied population, intubation time, timing or different intervals of endoscopic studies, and specially the difficulty in performing FLTB in ICU coma patients who have restrictions to exposing the larynx. Benjamin(1) used a routine direct laryngoscopy, under general anesthesia, in all patients with PTI in order to precisely diagnose and provide cleaning treatment of lesions and resections of granulation tissue.
Correlation of initial classes and variables (potential predisposing, triggering and aggravating factors)
Lindholm13, Donnelly7, Stauffer15, Kastanos11 and Colice5 did not find a correlation between age and severity of laryngeal lesion. In our series, advanced age was correlated with severe lesions.
Donnelly7 and Kastanos et al.11 did not find correlation with gender. In our series, we identified statistically significant difference in moderate class and male patients.
Lindholm13, in his study, could not statistically correlate motor activity - consequently, laryngeal activity of patients, and severity of laryngeal damage.
Colice et al.5 found correlation between presence of neuromotor activity and moderate and severe lesions at the initial assessment. Mackenzie14 and Lesnik et al.12 demonstrated higher incidence of laryngeal damage in patients with motor activity, restlessness and lack of sedation or with movement of decerebration and decortication.
The presence of neuromotor activity was not statistically significant. Absence of neuromotor activity, differently from what the literature says, was associated in our series with greater laryngeal damage, which posed conflicting information because the tube moved less inside the larynx.
Insufflated cuff in the trachea remained relatively fixed in a specific area. Neck flexion mobilized the tube 6cm inside the larynx, leading to more intense friction of glottic structures. Lateral movement, cough movement, swallowing, sneezing and movement generated by mechanical ventilation cause the same effect, leading to increase of area and severity of ischemia5.
In patients with Glasgow score up to 7, there was significance for the severe class. We did not find in the literature reference to Glasgow score and classes of laryngeal lesions after PTI.
Capillary perfusion of laryngeal or tracheal mucosa decreases as a result of chock hypotension, sepsis, hemodialysis and extra-body circulation, resulting in ischemia and laryngeal damage.
Colice et al.5, Thomas et al.(16) and Mackenzie14 did not find correlation between chock and severity of lesions or progression to laryngeal sequelae. Severe class was contradictorily associated with normal levels of arterial blood pressure. There was no statistically significant difference for presence of hypotension (p>0.05).
Stauffer et al.15 and Kastanos et al.11 did not find correlation between presence of respiratory infection and severity of laryngeal damage.
Laryngeal lesions were less severe if there were no tracheobronchopulmonary infections during the period of PTI. Tracheobronchopulmonary infections during intubation were correlated with higher rates of laryngeal damage. Absence of bronchial aspiration was significant for severe class (p < 0.001), opposed to what was expected, since bronchial aspiration is correlated with aspiration of gastric acid content and high rates of tracheobronchopulmonary infections - two factors that may increase the rate of laryngeal damage.
Chronic obstructive pulmonary disease or pulmonary diseases that produce mucus may increase the likelihood of laryngeal trauma, since the indications for mechanical ventilation support, tracheobronchial cleaning and bronchoaspiration have been expanded to patients with mucus hypersecretion or presence of pus13. Chronic and debilitating states, such as anemia, hypoproteinemia, diabetes, prolonged use of corticoids and alcohol abuse, affect the healing process and increase the incidence of complications10. El Naggar et al.8 did not find correlation of laryngeal lesions and other types of diseases.
Stauffer et al.15 and Kastanos et al.11 did not find correlation of laryngeal lesions caused by PTI and use of corticoids. In our series, we studied only assessment of cranioencephalic trauma. Other diseases or lesions were not assessed because of the reduced number of cases. There was statistically significant difference between cranioencephalic trauma and moderate class.
Friedman et al.9 reported three cases of patients whose nasogastric tube led to laryngeal alteration, causing intense arytenoid edema and ulcer with exposure of cricoid cartilage. The authors warned that the tube should not remain in median laryngeal position, and if so positioned, it should be replaced. The considerable absence of mucosa on the cricoid posterior region and the rigidity imposed by the cervical column and cricoid cartilage contribute to ulcer formation.
All patients in the present study maintained nasogastric tube during intubation time, therefore, it did not allow us to conclude which tube - tracheal or nasogastric - caused the laryngeal trauma.
Resolution time of laryngeal damage in group II
Evaluation of resolution time is difficult, since it requires repetitive endoscopies to observe evolution of lesions. Few studies provide this kind of data.
Lindholm13 described resolution time within 30 days for 45 patients (65%) out of 69, and resolution time within 60 days for 10 patients (14.5%), that is to say, within 60 days, 79.5% of the patients had normal larynxes.
Colice4 reported resolution time of 30 days after extubation in 31 (63%) out of 49 patients. Eleven patients (22.7%) had resolution time within 60 days. Within 60 days, 42 (85.7%) of the patients had a completely recovered larynx. In 80% of the patients, laryngeal lesions healed within 60 days, and there was a clear correlation between resolution time and initial classification: in 60% for mild class and in 36.8 % for moderate class, resolution time was 28 days; in 20% for mild class and in 42.1% for moderate class, it was from 29 to 60 days.
Resolution time in our series increased significantly as a result of tracheotomy and length of hospital stay (p=0.0052) and (p=0.0026), respectively. However, the duration of mechanical ventilation did not present statistical significance compared to resolution time.
Evolution f laryngeal lesions caused by PTI after tracheotomy
Burns et al.9 and Lindholm13 studied patients who had PTI followed by tracheotomy; however, they did not separate the data from patients submitted to PTI only.
PTI for more than 10 days followed by tracheotomy, in the presence of severe laryngeal lesion at extubation, does not influence laryngeal healing5.
Using the average scores of laryngeal lesions from patients during protocol FLTB (Chart 2), we clearly demonstrated that there was a decrease in mean scores of patients in group II with tracheotomy and extubated patients; within two months, the mean for patients without tracheotomy is zero, whereas the mean for patients with tracheotomy is four. There is, therefore, delay in healing time of lesions in patients with tracheotomy; in other words, they take longer to reach score zero. It is important to mention, though, that score zero refers almost always to presence of hyperemia only.
In Table 5, we observed that the mean scores of lesion for group II patients with tracheotomy and group I patients with tracheotomy were similar. There was no statistically significant difference to confirm that the disease or trauma severe enough to lead the patient to death had been responsible for delaying the regression of laryngeal lesions in these patients. Therefore, the healing process of laryngeal lesions progressed, even among those who eventually died.
The percentage of patients whose laryngeal lesions remained unaltered or improved after tracheotomy was 93% in group II and 89% in group I, with no statistically significant difference between the two groups (p<0.05). The percentage of patients whose laryngeal lesions worsened after tracheotomy was 7% in group II and 11% in group I.
Therefore, we noticed delay in resolution time in patients who had tracheotomy; however, after PTI, tracheotomy did not worsen laryngeal damage.
CONCLUSION
Acute laryngeal lesions by prolonged tracheal intubation (PTI) on the 6th day were present in all patients.
The resolution time of laryngeal damage was within 60 days in 80% of the patients, and there was a clear correlation with the initial class of lesions.
Tracheotomy did not aggravate laryngeal lesions caused by prolonged tracheal intubation, and 91.4% of patients improved or showed unaltered pattern of lesions after tracheotomy.
Predisposing, triggering and aggravating factors influence differently onset and severity of laryngeal lesions after prolonged tracheal intubation.
REFERENCES
1. BENJAMIN, B. - Prolonged intubations injuries of the larynx: endoscopic diagnosis, classification, and treatment. Ann. Otol. Rhinol. Laryngol., 102 (Suppl 160): 1-15, 1993.
2. BISHOP, M. J.; WEYMULLER, E. A.; FINK, B. R. - Laryngeal effects of prolonged intubation. Anesth. Analg., 63: 335-42, 1984.
3. BURNS, P H.; DAYAL, V S.; SCOTT, A. et al Laryngotracheal trauma: observations on its pathogenesis an its prevention following prolonged orotracheal intubation in the adult. Laryngoscope, 89: 1316-25, 1979.
4. COLICE, G. L. - Resolution of laryngeal injury following translaryngeal intubation. Am. Rev. Respir Dis., 145: 36164, 1992.
5. COLICE, G. L.; STUKEL, T. A.; DAIN, B. - Laryngeal complications of prolonged intubation. Chest, 96: 877-83, 1989.
6. DIXON, T C.; SANDO, M. J. W; BOLTON, M. J. et al. - A report de 342 cases of prolonged intubation. Med. J. Aust., 12: 529-33, 1968.
7. DONNELLY, W H. - Histopathology of endotracheal intubation. Arch. Path., 88: 511-20, 1969.
8. EL-NAGGAR, M.; SADAGOPAN, S.; LEVINE, H. et al. Factors influencing choice between tracheotomy and prolonged translaryngeal intubation in acute respiratory failure: a prospective study. Anesth. & Analg., 55: 195-201, 1976.
9. FRIEDMAN, M.; BAIM, H.; STOBINICKI, M. et al. Laryngeal injuries secondary a nasogastric tubes-Am. Otol., 40: 469-74, 1981.
10. IMBELONI, L. E. - Complicações da entubação traqueal. Rev. Bras. Anest., 36: 501-08, 1986.
11. KASTANOS, N.; MIR6, R. E.; PEREZ, A. M. et al. Laryngotracheal injury due to endotracheal intubation: Incidence, evolution, and predisposing factors. A prospective long-term study. Crit. Care. Med.. 11: 362-7. 1983
12. LESNIK, L; RAPPAPORT, W; FULGINITI, J. et al. - The role of early tracheotomy in blunt, multiple organ trauma. Am. Surg., 58: 346-9, 1992.
13. LINDHOLM, C. E. - Prolonged endotracheal intubation. A clinical investigation with special reference to its consequences for the larynx and trachea and to its place an alternative to intubation through a tracheotomy. Acta Anaesth. Scand., 33: 1-131, 1969.
14. MACKENZIE, C. F. - Compromises in the choice of orotracheal or nasotracheal intubation and tracheotomy. Heart & Lung, 12: 485-91, 1983.
15. STAUFFER, J. L.; OLSON, D. E.; PETTY, T. L. Complications and consequences of endotracheal intubation and tracheotomy: a prospective study of 150 critically ill adult patients. Am. J. Med., 70: 65-75, 1981.
16. THOMAS, R.; KUMAR, E. V; KAMESWARAN, M. et al. Post intubation sequelae in an intensive care unit. J. Laryngol. Otol., 109: 313-316, 1995.
17. VIA-REQUE, E.; RATTENBORG, C. C. - Prolonged oro or nasotracheal intubation. Crit. Care Med., 9: 637-39, 1981.
18. WHITED, R. E. - A prospective study of laryngotracheal sequelae in long-term intubation. Laryngoscope, 94: 367-77, 1984.
* Head of the Service of Thoracic Surgery and Respiratory Endoscopy at Hospital Universitário Cajuru - PUC - Curitiba /PR.
** Resident in Thoracic Surgery, Service of Thoracic Surgery and Respiratory Endoscopy at Hospital Universitário Cajuru (PUC-PR).
Affiliation: Hospital Universitário Cajuru (PUC-PR) - Avenida São Jose, 300 - 80050-000 Curitiba /PR.
Address correspondence to: Clínica do Tórax - Avenida Comendador Franco, 2429 - 81520-000 Curitiba /PR - Brazil - Tel: (55 41) 266-3500 / Fax: (55 41) 266-4349.
Article submitted on July 12, 2000. Article accepted on February 9, 2001.