Year: 1996 Vol. 62 Ed. 6 - (1º)
Artigos Originais
Pages: 459 to 462
The Value of Neck Torsion Nystagmus in Neurootologic Evaluation.
Author(s):
Maudonnet O, MD*,
Gutierrez F, MD**,
Bilecki M, MD**.
Keywords: Neck torsion nystagmus, neurootologic evaluation
Abstract:
Neuro-otologic evaluation was performed in 502 patients, emphasizing the test on neck torsion nystagmus because it was very controversial. Patients were divided into three groups: no labyrinth and cervical symptoms, no labyrinth symptoms with cervical symptoms and labyrinth and cervical symptoms. In the first group, we did not find any neck torsion nystagmus; in the second group, two patients (2.17%) had it, and the third group showed all possible results: neck torsion nystagmus was absent in 66 (21.85%) individuals, in 129 (42.79%) it was degree 1, in 96 (31. 79%) it was degree 2, and in 11(3.64%) it was degree 3. Analyzing the abone results, we conclude that neck torsion nystagmus is retevant in the study of patients with vestibular symptoms. As there is no conclusive signal in neuro-otology, its high frequency in patients with cervical syndrome is quite an important point iu its diagnosis.
![]()
INTRODUCTION
In 1907, Bárány described the existence of extravestibular nystagmus that raised when body rotation was promoted, with head standing immovable. In 1967, Greiner and col. settled the bases of its physiopatology and determined its clinical application. According to these authors, neck torsion nystagmus is an extravestibular response due to the transmission of a proprioceptive influx arising from articular capsulas and from the ligaments of the first three cervical vertebrae. This impulse would be transmitted by spino-vestibular tract until reaching inferior vestibular nuclei in the fourth ventricle. Also according to these authors, this impulse would be antagonistic to the vestibular ones, what would explain its enhancement in cases of total bilateral peripheral vestibular injury, as in ototoxicosis. Nystagmus' research takes approximately two minutes and should be carried out in a dark and soundless room. Body rotation should be done manually, around 60° to the right and to the left, maintaining head steady. Initially, rotation should be slow, after 20 seconds it is repeated to the opposite side; then a new rotation is done, now with rapid movements in both directions. Responses are easily interpreted, since neck torsion nystagmus has an opposite direction to the pendular rotatory test. According to the intensity, its evaluation should be: 0, when it is absent; 1, when there is nystagmus only during rapid movements; 2,when they are present in rapids and slow movements; 3, when they persist while positionis maintained.
In 1969, Thiébaut demonstrated that patients with vertebro-basilar insufficiency have normal arteriographies when neck torsion nystagmus is absent. In 1977, Boniver concluded that the presence of neck torsion nystagmus leads us to think about a cervical column problem, but he does not explain whether it is caused by a stenosis of vertebral arteries or by an impulse disorder of muscular origin. According to Maudonnet (1977), there is a correlation between the intensity of neck torsion nystagmus and the radiological changes. Thus, degree 2 and 3 nystagmus are always associated with important alterations in the cervical column, mainly regarding conjugation foramens.
In 1969, Greiner e col. showed that normal individuais did not present neck torsion nystagmus, corroborated by Coilard and col. (1973). However, in 1976, Norré and col. found it in 57.1% of normal subjects and, in 1978, Depond in 11.09%. These apparently contradictory results caused a great controversy about the value of neck torsion nystagmus. Some authors just do not research it, while others still believe its responses are effective. The aim of our research is trying to elucidate this polemical matter, to know how important this test is in neurotologic evaluation.
METHODOLOGY
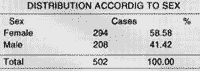
We studied 502 patients, 294 female (58.58%) and 208 male (41.42%).
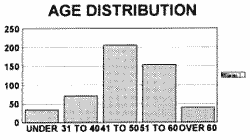
Ages ranging from 28 to 67 year old. Is is more frequent in the forties (Fig. 1).
All individuals were submitted to a complete neurotologic evaluation, including the research of neck torsion nystagmus . They were divided into three groups:
A - no vestibular and cervícal symptoms.
B - no vestibular symptoms, but with cervical symptoms (cervical pains spreading to the back and shoulders, limited head movement, snaps due to head rotation, paresthesia in upper limbs etc).
C - cervical and vestibular symptoms (rotatory vertigo, mainly due to abrupt head movement, being more intense in the morning when waking up; periodical crises of a feeling of fluctuation, lability, tinnitus etc).
Figure 1.
All of them were submitted to anamnesis, otorhinolaryngologic and cervical column examinations, audiometric and vestibular tests, including the research of neck torsion nystagmus. As many patients showed limited head movements, we decided for its manual fixation and chair was also manully rotated, with a maximum displacement of 60° and a minimum of 35°. First rotation was to the left, lasting approximately 20 seconds, followed by a 20 seconds stop at the position of maximum torsion and then by a rotation to the right in the same conditions. The procedure is repeated 3 times. So the whole testing takes about 240 seconds.
The responses of Group C were evaluated by using the classification of Greiner and col. 1977, with some modifications:
Degree 0 - absence of nystagmus.
Degree 1 - nystagmus arises only during chair rotation, with minimum frequency ( two to five beats).
Degree 2 - nystagmus is present during rotation and remains for some more seconds after chair stops.
Degree 3 - similar to the former, but it remains beating all the time.
RESULTS AND DISCUSSION
Neck torsion nystagmus was absent in all 108 patients of group A, i.e., with no vestibular and cervical complaints, corroborating the findings of Greiner and col. in 1967. We observed in the course of the research that patients moved their head during the test, some in the direction of chair rotation ( failure in fixation or patient's own movement) which was easily perceived because nystagmus beat in the opposite direction to that of cervical origin. However, several patients, perhaps anxious for helping the examiner, rotated the head inversely to the chair, causing a small per-rotatory nystagmus, being similar to a nystagmus of cervical origin and hardly differentiated when only tracing is considered. We found out such irregularity by observing our technician during the test, which is completely imperceptible to her. This kind of nystagmus was found in 18 patients (16.66%): in 14 (12.96%) it was a degree 1 cervical pseudo-nystagmus and in 4 (3.70%) it was degree 2. Rather than attributing the apparently incongruent results of the incidente of neck torsion nystagmus to this technical failure, we intend to alert to its possible incidente and in our opinion, this kind of nystagmus requires further researches.
Regarding group B, composed by 92 subjects, neck torsion nystagmus was shown in only two cases degree 1 (2.17%). As we believe they are probable carriers of future cervical syndromes, they have been followed-up. Up to the date of this work's conclusion, they did hadn't any cochlearvestibular symptoms.
The table below relates the results of Group C:
The analysis of the above result indicates that neck torsion nystagmus may be absent in patients with confirmed diagnosis of cervical syndrome, corroborating researches of Norré and col., in 1976. Identically, degree 1 and 2 were also the most frequent ones. Degree 3, less frequent, was usually associated to a more severe pathology identified by the patients complaints and by the electronystagmographic findings.
It was not possible to correlate the presente of neck torsion nystagmus with the etiology of cervical syndrome (osseous, articulatory, muscular or vascular pathology), in any of the cases, what corroborates the researches of Collard and col. (1973) and Boniver (1976).
CONCLUSION
Although the research of neck torsion nystagmus is simple and rapid, it requires certain precautions to avoid pseudo-cervical nystagmus to come out.
It is absent in normal individuals and in those with cervical pathology with no involvement of cochlearvestibular system.
The presente of nystagmus is not obligatory in cervical syndrome.
When present, it does not reveal the etiology of this disease, serving just as an orientation for a cervical problem.
REFERENCES
1 - BARANY R. - Nistagmusanfälle nach Kopfbewegungen bei Fällen mit Schwindel ohne Zertstörung des Vestibularapparates. Mschr. Ohren Heilk; 510,40-46, 1907.
2 - GREINER G., CONRAUX C. & COLLARD M. - Véstibulométrie Clinique.Doin Ed. Paros, 1969. 177-179.
3-THIÉBAUT F.- Valeur respective des renseignements fournis par l'angiographie vertébrale dynamique et la recherche d'un nystagmus d'origine cervicale dans l'insuffisance vertébro-basilaire. Rev. Neurol.; 41, 167-172, 1969.
4 - BONIVER R. - Le vertige d'origine cervicale. Rev. Medicale de Liege; 245,
31-37, 1976.
5 - MAUDONNET O. - Sindrome Cervical - a propósito de 166 casos. Rev Bras. de
ORL; 43, 258-261. 1977.
6 - GREINER G, CONRAUX C. & THIEBAUT M. - Le nystamus d'origine cervical Rev. Neurol; 117, 677- 682, 1967.
7 - COLLARD M., CONRAUX C & WATERS J. - Les syndromes vestibulalres centraux. Paris, Masson Ed. 1973, 114-115.
8 - NORRÉ M. & STEVENS A. - Le nystagmus cervical et les troubles fonctionnels de la colonne cervicale. Acta Otorhinolaryngol. Belg.; 30, 457-467, 1976.
9 - DEPOND M. - Le nystagmus d'origine cervicale. Acta Otorhinolaryngol. Belg.; 28, 759-760, 1974.
* Professor de Otoneurologia da Faculdade de Ciências Médicas da Unicamp.
** Prof. Voluntários de Otoneurologia da Faculdade de Ciências Médicas da Unicamp.
Trabalho realizado na Clínica de Otoneurologia da F.C.M. da Unicamp e no Instituto Penido Burnier.
Paper presented at the 23th NES Congress - Bad Kissigen - Germany - March 1996.
Endereço - Av Andrade Neves 611, 13013-161 - Campinas - Fone - (019) 2361027 - Fax - (019) 233 1265
Artigo recebido em 12 de março de 1996.
Artigo aceito em 26 de abril de 1996.