IntroductionDystonias are neurological disorders of central motor processing characterized by abnormal or involuntary movements or uncontrollable spasms induced by activity. These movements can occur at any body region and are aggravated by fatigue, stress and emotions. Dystonia is most of the times idiopathic, but it can be secondary to other disorders. In children, symptoms are normally focal at the onset, followed by generalization to other parts of the body, whereas in adults, symptoms are normally focal and so remain 1. In 1982, Marsden and Sheehy reported the correlation between Meige's syndrome (blepharospasm and oropharyngomandibular dystonia) and dystonic torticollis and laryngeal dystonias 2.
Laryngeal dystonias are classically classified into two types, both characterized by changes in vocal quality: adductor dystonia, also called spasmodic dysphonia, and abductor dystonia. Both are due to spasms of the respective laryngeal muscles during speech, being considerably less impaired during laugh, singing, cough, whispering and falsetto 3 , with no impairment of the respiratory laryngeal function. In adductor dysphonia, voice is tense and strained, with frequent vocal breaks and vocal stress. In abductor dysphonia there is intermittent vocal breathiness, prolongation of voiceless consonants and vocal breaks with aphonia. Brin and Blitzer, in 1991, identified a third type of laryngeal dystonia named breathing laryngeal dystonia (BLD), in which the abnormality affected the laryngeal breathing function 4. Later, other authors reported similar cases 5, 6. Breathing laryngeal dystonia (BLD) is a rare disorder in which the patients present persistent inspiration stridor, inappropriate respiratory pauses and absence of dysphonia. The examination of these patients shows presence of paradoxical vocal fold motion (PVFM) during inspiration. Stridor normally disappears during sleep and worsens with stress and most patients do not present desaturation of arterial oxygen. There may be difficulties in swallowing owing to lack of coordination between breathing and swallowing. Many patients present other focal dystonias such as blepharospasms, mandibular dystonia, torticollis, or upper limb tremor. Head trauma and degenerative disorders such as multiple systemic atrophy and amyotrophic lateral sclerosis has also been associated with this disorder 7. Laryngeal electromyography is useful in diagnosing laryngeal dystonia, being that the most common findings are: extended potentials, polyphasic potentials and irregular tremor. Other common abnormalities include small potentials, reduced number of motor units, regular tremor, dennervation potential, pseudomyotonic discharges and voluntary activity breaks 1. Botulinum toxin is the most effective treatment described for spasmodic adduction dysphonia and treatment for abduction dystonia is still controversial 8. Anticholinergic drugs 1 and applications of botulinum toxin in one or both posterior cricoarytenoid muscles 6 are the treatment proposed for this disease. Many treatment approaches have been tried for BLD but with little success. The use of Botox® in the thyroarytenoid muscle has provided some promising improvement, despite the few reported cases 5. Botulinum toxin is produced by the bacterium that causes botulism, Clostridium Botulinum. There are at least 7 types of serologically different toxins produced by the bacterium, all of them extremely powerful neuroparalytic agents, being neurotoxin A the most powerful one. When injected in minimum doses, botulinum toxin blocks the discharge of acetylcholine in neuromuscular joints and provokes selective muscle hypotonia that leads to flaccid paralysis 4, which is extremely convenient to patients who have phonation and breathing spasms 4. The paralysis generated by Botox is transient and lasts about 6 months and the side effects are minimum: breathiness and some difficulty to swallow in the first two weeks. Koufman and Blabock, in 20026, after clinical laryngostroboscopic and electromyography exams of 100 patients with laryngeal dystonia concluded that the traditional classification of focal laryngeal dystonia into adduction/abduction represented a very simplified way of classifying them, and proposed another classification with 10 subtypes of laryngeal dystonias, including BLD, which facilitates diagnosis and predicts the response to treatment with Botox. The authors analyzed 200 cases according to the proposed classification and the results were: adductor dystonia (glottic, supraglottic, dystonic tremor, adduction with tremor) - 80%; pure adductor dystonia (glottic) - 41%; abductor dystonia - 4%; mixed dystonia (abduction, with compensation of adductor component, adduction with compensation of abductor component, abduction with tremor) - 11%; breathing dystonia - 2%; non-focal dystonia (Meige's syndrome, cerebral palsy, etc.) - 3%. In laryngeal focal dystonia of supraglottic adduction, speech fluency is more severely affected; paradoxical motion closes the endolarynx, which has a sphincter appearance, and patients with this type of dystonia respond to Botox®. In dystonic tremor, glottic hyperabductions are rhythm and absent during breathing and patients do not respond that well to treatment with Botox® as other laryngeal dystonias. Abduction dystonia with compensation of adductor component has a marked expression of the abductor component after the injection with Botox® in the thyroarytenoid muscle and the voice remains dystonic and with further breathiness.
In the present article we present two clinical cases of patients with BLD treated with Botox that presented inspiration glottic closure caused by anomalous spasms of thyroarytenoid and lateral cricoarytenoid muscles, such as paradoxical epiglottis motion.
Objectivve
The purpose of the present article was to discuss clinical, laryngological and electromyography factors that supported the diagnosis of breathing laryngeal dystonia (BLD) by reviewing the current concepts in laryngeal dystonias. It also intended to include, in the classification proposed by Koufman and Blabock to laryngeal dystonias, a new subtype of BLD in which there is posterior flexion of the epiglottis, followed by its suggested therapeutic approach.
Methods
We reported two cases of patients with dyspnea with suspected diagnosis of breathing laryngeal dystonia. The patients underwent clinical history and nasofibrolaryngoscopy to assess functionally larynx and pharynx from a phonation and respiration perspective; telelaryngoscopy to observe the abnormalities in the cover layer of the vocal folds and the rest of the larynx with electromyography to have a functional assessment of the various laryngeal muscles. Next, we presented the therapeutic management to which the patients were submitted and their outcomes. The clinical findings of the patients were compared with the findings in the literature resultant from a Medline data survey.
CASE REPORTCASE 1
Male 21-year-old Caucasian patient, coming from Rio de Janeiro, with history of dyspnea for one year, without correlation with physical stress. The patient did not report vocal complaints, choking, gastroesophageal reflux or abnormal motion of any body parts. He did not report family history of dystonia or other neurological diseases. Nasofibrolaryngoscopy showed base of the tongue placed posteriorly and epiglottis malacia; telelaryngoscopy did not show any abnormalities. We conducted lingual tonsillectomy and partial removal of the epiglottis, with no improvement of the condition. In a new examination, we detected paradoxical laryngeal movement, with glottic closure at the end of inspiration, followed by pharyngeal closure. Larynx electromyography evidenced the electrical activity of adductor muscles (thyroarytenoid and lateral cricoarytenoid) during inspiration. We injected 10 units of botulinum toxin (Botox®) in the thyroarytenoid muscle on the left under electromyography control. Since the patient reported no significant improvement, 15 days later, we had a new injection of 10 units of Botoxâ in the lateral cricoarytenoid muscle on the same side. The patient was asymptomatic for 5 months, when other 10 units of Botox® were injected in the left thyroarytenoid and lateral cricoarytenoid muscles. Since there was persistence of partial dyspnea, we injected 10 more units of Botox® in the contralateral thyroarytenoid muscle. The patient remained well for more 6 months when once again he required therapy with botulinum toxin. At that time, we injected 10 units in both thyroarytenoid muscles and in the left lateral cricoarytenoid muscle, and he has currently been asymptomatic for 5 months.
CASE 2
Male 55-year-old Afro-descendent patient, coming from Pernambuco and living in Sao Paulo for over 31 years, security guard, former smoker, complaining of dyspnea for 1 year associated with inspiration and expiration stridor. The patient reported exacerbation of symptoms in moments of anxiety. He did not report vocal complaints, choking, symptoms of gastroesophageal reflux or abnormal motion of the body parts. He also did not report family history of dystonia or other neurological affections. Nasopharyngolaryngoscopy showed that during inspiration the patient had retro-positioning of the tongue base, paradoxical vocal fold motion and epiglottis flexed posteriorly, contributing to stridor (Figure 1). This flexion of the epiglottis cartilage was followed by a movement of tongue anteriorization and elevation of epiglottis. Telelaryngoscopy did not evidence other abnormalities. Polysomnography showed level of apnea/hypoapnea within the normal range and we did not observe the presence of laryngeal stridor during sleep and the patient maintained basal saturation of oxyhemoglobin of 95%. Laryngeal electromyography showed presence of recruiting of bilateral adductor muscles (lateral cricoarytenoid and thyroarytenoid) during inspiration. We injected 5 units of Botox® in the left thyroarytenoid muscle. After application, the patient referred improvement of vocal breathiness and choking with liquids, which persisted for two weeks. The patient presented partial improvement of the condition since there was persistence of paradoxical epiglottis motion during inspiration. We decided to cause paralysis of the muscle responsible for the posterior flexion of the epiglottis and the patient was submitted to application of 10 units of Botoxâ in the right aryepiglottic wall (Figure 2) with reduction of episodes of abnormal epiglottis movement and significant improvement of breathing condition (Figure 3).
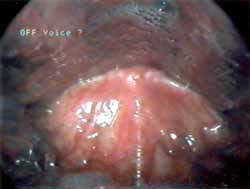
Figure 1. Posterior flexion of the epiglottis during inspiration.
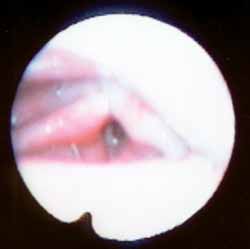
Figure 2. Botox® injection, direct aryepiglottic wall, transluminar transcutaneous access.
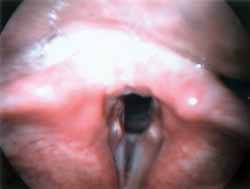
Figure 3. Absence of paradoxical vocal fold motion and epiglottis during inspiration after injection of Botox® in the thyroarytenoid muscle and aryepiglottic wall.
Paradoxical vocal fold motion (PVFM) is characterized by inappropriate adduction of the vocal folds during inspiration. Despite the fact that the adduction muscles are normally activated during inspiration, the contraction of these muscles in PVFM is very significant, such as observed in the EMG of these patients, leading to inspiration stridor. Multiple causes have been referred in the literature for PVFM, being that BLD is one of them 7. Thus, the assessment of these patients requires identification of the etiology in order to direct the complementary investigation and the appropriate management. However, the etiological diagnosis of dyspnea condition can be difficult to be made, especially because many times these patients are in emergency situations, being that BLD is probably more frequent than the number of cases described. In fact, many cases of inspiration stridor caused by glottic opening reduction were attributed to bilateral vocal fold paralysis in adduction by paralysis of the abductor muscles, a condition named Gerhardt's syndrome. Marion et al., in 1992, however, reported electromyographic findings of 6 patients with previous diagnosis of Gerhardt's syndrome that had normal activity of the adductor muscles and spasms of the thyroarytenoid muscles during inspiration 6. Thus, this condition represents in reality laryngeal focal dystonia, with involuntary hyperactivity of the adductor muscles and not paralysis of the abductor muscles as previously proposed. The literature also brings some reports of patients with stridor without identifiable organic causes, diagnosed as functional disorders (conversion reaction) caused by abnormal motion of the vocal folds 8. This disorders was called Munchausen's stridor 10. Chistropher et al., in 1983, described 5 patients with paradoxical dyspnea and primary diagnosis of severe asthma, which persisted after asthma management 12. These patients did not present evidence of lower airway obstruction after the conduction of complementary investigation, and when symptomatic, the laryngoscopy findings were complete adduction of the vocal folds and partial adduction of the vestibular folds, but with arytenoid cartilages maintaining the lateral position, leading to the formation of a wide posterior triangular chink. It was diagnosed in these patients a wide range of psychiatric disorders that varied from stress related to exacerbation to symptoms of obsessive-compulsive disorders. Abnormal vocal fold motion was not seen when the patient was asked to make it consciously, leading to the conclusion that those abnormal movements were a somatic unconscious expression of dysphoric feelings, with typical characteristics of conversion disorders and these patients were successfully treated with psychotherapy associated with speech and voice therapy. The author concluded that this functional disorder should be part of the spectrum of breathing disorders related to laryngeal abnormalities. Maschka et al., in 1997, proposed a classification for the paradoxical vocal fold motion grouping the causes of PVFM in two groups: organic causes (cortical or upper motor neuron lesion, nuclear or lower motor neuron lesion, movement disorders or gastroesophageal reflux) and non-organic causes (somatization disorder, conversion or malingering) 7. Organic causes of PVFM are less frequent than non-organic causes. Gastroesophageal reflux is normally present in patients with PVFM even though the correlation between cause and effect has not been well established for these disorders yet. We may find PVFM during an episode of gastroesophageal reflux as well as gastroesophageal reflux during an episode of PVFM, owing to increase in intrathoracic inspiration negative pressure.
Patients with pictures of brainstem compression (for example, Arnold Chiari's malformation, cerebral aqueduct stenosis, arachnoid cyst in the posterior fossa) are rarely described in the literature 7 and by compression of the ambiguous nucleus, they present other manifestations of vagal dysfunction such as velopharyngeal incompetence, dysphagia and gastroesophageal reflux. These disorders can be diagnosed by magnetic nuclear resonance and require neurosurgical intervention that normally normalizes the vocal fold movement. Patients with PVFM attributed to severe cortical dysfunction after cerebral vascular accident present multiple neurological abnormalities, as well as children and adolescents with non-progressive encephalopathy that present delay of neuropsychomotor development and nasal or oropharyngeal obstruction. PVFM resultant from recurrent nerve lesion is rare in the absence of brainstem compression, but it has been described in patients with amyotrophic lateral sclerosis, myasthenia gravis and medullary infarction. PVFM can also be present in patients with motion disorders such as breathing laryngeal dystonia (BLD), myoclonus, Parkinson's disease and Parkinsonism secondary to neuroleptic use. Non-organic causes of PVFM have innumerous denominations such as psychogenic stridor and Munchausen's syndrome and they are normally present in young women who frequently have previous diagnosis of psychological disorders. These patients improve during sleep and the vocal folds adduct correctly during cough and Valsava's maneuver. They can still present breathy vocal quality.
Whereas PVFM is consciously produced by malingering patients motivated by secondary gains obtained with the attention evoked by these patients during the episodes of dyspnea, patients with conversion disorders presented non-intentional PVFM. The treatment is conducted with psychotherapy and voice therapy to reduce laryngeal muscle tension, reduce vocal hyperfunction and improve breathing control. Grillone et al.10 studied 7 patients with diagnosis of BLD and observed that 33% of the patients were women and 67% were men, whose mean age at the onset of symptoms was 33 to 62 years, mean of 49.1 years and no family history. All patients presented at the beginning of laryngeal manifestations or during the disease some other dyskinesia with oromandibular dystonic motion, tongue, blepharospams or tremor. The distribution concerning gender and family history of these patients differed from the findings observed in laryngeal dystonia that impaired phonation. Blitzer and Brin, in 1988, in a study involving 110 cases of laryngeal focal dystonia with phonation impairment, observed a proportion of 1.4 women to each men and positive family history of 23% 1. The mean age at the onset of symptoms was 34.6 years, other dystonic manifestations were seen at 48% and associated tremor in 29% of the patients1, representing common characteristics of phonation and respiration types of laryngeal dystonia. Speech therapy, psychotherapy, pharmacotherapy with benzodiazepinic drugs, anticholinergic and anti-dopaminergic drugs have been the treatment approach used with BLD but the result are limited. Grillone et al., motivated by the success described with Blitzer and Brin in the treatment of adduction laryngeal dystonia with application of toxin botulinum type A in thyroarytenoid muscle 1 and with the initial promising reports of BLD treated with BOTOX® 4, 6, applied in their patients, in both thyroarytenoid muscles, injections of toxin type A reconstituted with saline solution in a concentration of 25 U/ml, with doses injected in the muscle ranging from 0.625 to 3.75U, according to the severity of stridor. All patients felt the effects of the toxin in the larynx 72 hours later, reaching the maximum effect within 2 weeks and the improvement was maintained for an average period of 13.8 weeks. The side effects included breathy voice and mild aspiration of liquids that reverted on average 2 weeks later.
Epidemiological data of the patients reported by us coincided with what is described in the literature for BLD being that both patients were male, adults and without family history of dystonia. Both patients presented episodes of involuntary adduction of the vocal folds during inspiration and normal muscle function during speech. This task-dependent motion disorder, confirmed objectively by electromyography, is a typical symptom of dystonia, as well as the exacerbation of the condition with emotional stress and its absence during sleep, as demonstrated by polysomnography of the second case described here. The patients did not present other neurological symptoms that pointed to cortical or brainstem disease or associated dystonic movements. The follow up of these patients in the long run is important so that we can assess the occasional onset of symptoms of degenerative diseases or other motion disorders, even though dystonias at the beginning of the adult age tend to remain focal. The two reported patients presented inspiration glottic closure caused both by anomalous spasms or thyroarytenoid muscles and lateral cricoarytenoid muscles, or by epiglottis paradoxical motion. Maschka et al. described a similar clinical case of a 14-year-old boy with episode of stridor and mild apnea associated with the presence of paradoxical vocal fold motion and epiglottis posteriorly turned, resulting from mild laryngomalacia 7. The author suggested that the Bernoulli's effect detected in the presence of inspiration with closed glottis can promote laryngomalacia and influence severity of PVFM and that patients with similar occurrences can benefit from the procedure that promote further patency of the airways (such as adenotonsillectomy and uvulopalatopharyngoplasty) by reducing Bernoulli's effect. Such opinion is not shared by us, since our first patient was submitted to lingual tonsillectomy and partial removal of the epiglottis and there was no improvement of the condition. We believe that paradoxical epiglottis motion is only one more dystonic manifestation characterized by uncontrollable spasms of the aryepiglottic muscle. This opinion is confirmed by the observation of improvement obtained by the second patient after the injection of Botox in the aryepiglottic wall. The classification of laryngeal dystonia proposed by Koufman and Blabock seems to be better than the traditional division of the disease into adductor/abductor, since it values the existence of mixed types of laryngeal dystonias and the concomitant presence of other motion disorders that can be found in clinical practice. Therefore, the clinical cases presented by us can be included in this classification, as a supraglottic subtype of breathing laryngeal dystonia, characterized by adduction paradoxical motion of endolarynx (true vocal folds, false vocal folds and supraglottic structures of the epiglottis), which takes on the sphincter appearance, such as during swallowing. We observed significant improvement of symptoms in our patients after application of Botox® in the adductor muscles, with few side effects.
ConclusionEtiological diagnosis of laryngeal stridor can be difficult to be made, especially because sometimes these patients are in emergency situations. Therefore, breathing laryngeal dystonia, one of the possible affections that cause paradoxical vocal fold motion, with clinical manifestations of stridor and dyspnea, can have even higher incidence than normally described. The diagnosis of BLD requires first of all complete medical history and laryngological and neurological examinations, focusing on checking the presence of dystonic characteristics and ruling out other etiologies that cause paradoxical vocal fold motion. Electromyography of the larynx can provide data about the activity of the laryngeal muscle group and it seems to the most useful additional exam in these cases. The use of Botox in adductor muscles of the vocal folds has provided significant improvement of symptoms in these patients, despite the few described cases. The classification of laryngeal dystonia proposed by Koufman and Blabock values the existence of mixed types of laryngeal dystonias and the concomitant presence of other motion disorders. The presence of paradoxical adduction motion of glottic and supraglottic structure characterized by posterior flexion of epiglottis during breathing, such as the clinical cases presented here, can be valued as a creation of a subtype of breathing laryngeal dystonia within this classification.
References 1. Blitzer A, Brin MF, Fahn S, Lovelace RE. Clinical and laboratory characteristics of focal laryngeal dystonia: study of 110 cases. Laryngoscope 1988; 98:636-40.
2. Marsden CD, Sheehy MP. Spastic dysphonia Meige disease and tortion dystonia. Neurology 1982; 32: 1202-3.
3. Shaefer SD. Neuropathology of spasmodic dysphonia. Laryngoscope 1983; 93: 1183-1204.
4. Brin M.F, Blitzer A, Braun N et al. Respiratory and Obstructive Laryngeal Dystonia treatment with Botulinum Toxin (Botox). Neurology 1991; 41(1):291.
5. Lew MF, Shindo M, Moskowitz C et al. Adductor laryngeal "breathing dystonia" in a case of x-linked dystonia-parkinson syndrome. Mov Disord 1992; 7:301.
6. Marion M, Klap PA, Cohen M. Stridor and focal laryngeal dystonia. Lancet 1992; 339: 457-58.
7. Maschka DA, Bauman NM, Mccray PB, Hoffman HT, Karnell MP, Smith RJH. A classification scheme for paradoxical vocal cord motion. Laryngoscope 1997; 107: 1429-35.
8. Behlau M, Pontes P. As chamadas disfonias espasmódicas: dificuldades de diagnóstico e tratamento. Rev Bras Otorrinolarigol 1997; 63 (Supl): 4-27.
9. Koufman JA, Blalock PD. Classification of laryngeal dystonias [monograph online]. North Carolina: Center for Voice Disorders of Wake Forest University. [citado 2002 Mai24]. Disponível em: URL: http:// www. bgsm.edu/voice/class ld.html
10. Grillone GA, Blitzer A, Brin MF, Annino DJ, Saint-Hilaire MH. Treatment of adductor laryngeal breathing dystonia with botulinum toxin type A. Laryngoscope 1994; 104: 30-2.
11. Patterson R, Schatz M, Horton M. Munchausen's stridor: non-organic laryngeal obstruction. Clin Allergy 1974; 4: 307-310.
12. Christopher KL, Wood RP, Eckert RC, Blager FB, Raney RA, Souhrada JF. VocCASE REPORTRELATO DE CASOal-cord dysfunction presenting as asthma. N Engl J Med 1983; 308: 1566-70.
1 Master studies under course, Discipline of Otorhinolaryngology, Escola Paulista de Medicina (UNIFESP-EPM).
2 Assistant physician, Division of Laryngology and Voice, Discipline of Otorhinolaryngology, Escola Paulista de Medicina (UNIFESP-EPM).
Physician with Instituto da Laringe (INLAR).
3 Intern physician, Discipline of Otorhinolaryngology, Escola Paulista de Medicina (UNIFESP-EPM).
4 Faculty Professor of Otorhinolaryngology, Full Professor, Escola Paulista de Medicina (UNIFESP-EPM).
Study conducted at the Division of Laryngology and Voice, Discipline of Otorhinolaryngology,
Escola Paulista de Medicina (UNIFESP-EPM)/ Instituto da Laringe (INLAR).
Address correspondence to: Mariana D.A. Lebl - Av. Higienópolis, 1048 apto. 126 São Paulo SP 01238-000
E-mail: marklebl@hotmail.com.
Article submitted on December 15, 2002. Article accepted on July 01, 2003.


