INTRODUCTIONInverted papilloma UP) is a true benign epithelial neoplasia with hyperplastic epithelium growth in the inner part of the underlying stroma1,4. Usually, it grows either in the middle meatus or in the nasal lateral wall and, very rarely, in the nasal septum and paranasal sinuses9. It accounts for 0.5 to 4% of all nasal tumors1.
Although it has a benign histology, IP can invade the bone walls of the paranasal sinuses spreading to the surrounding tissues1,9. They may become malignant and recurrence rates range from 0% to 78%10.
According to Sham et al.13, surgical treatment may be the following:
1. Non-endoscopic nasal approach: polipectomy or sphenoethmoidectomy.
2. Limited extranasal approach: Caldwell-Luc operation or external ethmoidectomy.
3. Radical extranasal approach: lateral rhinotomy or degloving with en bloc resection of the lateral wall.
4. Endoscopic endonasal, resection.
The present study aims at reviewing clinical and surgical findings on patients suffering from nasal or paranasal sinuses inverted papillomas, who have been treated at the Hospital do Servidor Público Estadual de São Paulo - Francisco Morato de Oliveira (HSPE-FMO).
MATERIAL AND METHODFrom August 1996 through July 2000, eight patients suffering from nasal or paranasal sinuses inverted papilloma were submitted to surgical treatment at HSPE-FMO. In retrospect, we have studied the following variables: age of patient at the time of diagnosis, sex, pre-operative symptoms, site of tumor, presence of associated inflammatory polyposis, surgical approach and chosen procedure, recurrence, development into malignancy and follow-up time after surgery. There were five male patients (62.5%) and three female patients (37.5%). Average age was 61.5 years (52 - 77 years of age) (Table 1).
RESULTSTable 1 shows patients listed according to sex and age.
Table 2 describes the pre-operative symptoms reported by the eight patients.
In Table 3 we see the localization of tumors: in five patients, the IP started in the lateral nasal wall (62.5%); in two patients, it started in the maxillary sinus (25%); in one patient it was located in the nasal septum. In all the cases the inverted papilloma attacked only one of the nasal cavities and three patients had an associated inflammatory polyposis.
Three of the patients (37.5%) were submitted to maxillary ethmoidal sinusectomy by means of a medial-facial degloving, and, in one of the cases the surgery was complemented with an external ethmoidectomy; three other patients (37.5%) were submitted to endonasal endoscopic resections, and, two patients (25%) underwent Caldwell-Luc operations. Follow-up time varied from one to 47 months, mean of 18 months (Table 3).
Table 1. Distribution of the eight patients with inverted papilloma according to sex and age.
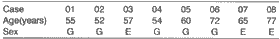
E= females. G= males.
Tabela 2. Sintomatologia pré-operatória dos oito pacientes portadores de papiloma invertido.

Table 3. Site of lesion, surgical approach used, presence of associated polyposis and post-operative follow-up in the eight patients with inverted papilloma.
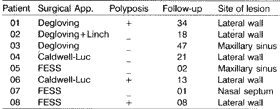
FESS = Functional endoscopy facial sinuses surgery.
Degloving = Middle facial degloving with maxilloethmoidal sinusectomy.
Linch = External ethmoidectomy by Linch incision.
+ = presence of associated polyposis
- = absence of associated polyposis
In none of the cases there was transformation into malignancy nor recurrence of the inverted papilloma.
DISCUSSIONInverted papilloma is a benign tumor of ectodermal origin, which stems from the nasal mucosa and the paranasal sinuses. The type of epithelium may be respiratory, transitional or squamous2,3,11. Some authors suggested that the infection by HPV (Human Papillomavirus) may be responsible for the development of the inverted papilloma2,3,11. Although the presence of HPV is not related to the increase in likelihood of transformation into a malignant kind, studies found that subtypes 6 and 11 were only observed in benign inverted papillomas, whereas subtype 16 was mostly found in lesions where there was a carcinoma8.
The highest incidence of inverted papilloma was among men, who showed unilateral nasal obstruction in their fifth or sixth decades of life, as disclosed by Lawson et al.9 in a series of 112 cases. Our study matched these findings, in which 62.5% of the patients were men with a mean age of 61.5 years.
Chee and Sethi5 described the cases of 18 patients with inverted papilloma, mean age 53 years: 78% of the patients were male and 22% were female patients.
Inverted papilloma is more frequently localized in the lateral nasal wall involving or spreading towards the paranasal sinuses and surrounding structures by direct extension12, which has corresponded to our findings, since 62.5% of the cases had its origin in the nasal lateral wall.
Some authors' first choice was a radical extranasal approach. Others recommend limited endonasal or extranasal approach13. Today, the standard procedure is a lateral rhinotomy; however, it has its disadvantages such as a facial scar, excessive resection of the normal mucosa and bone tissue, as well as a possible injury to the nasolachrymal duct. The medial facial degloving procedure avoids the facial scar but can cause vestibular stricture, epiphora, subcutaneous hematoma and facial dysesthesia, and, besides, it does not allow a broad access to the frontal sinus9.
With the introduction of endoscopes, we can perform wider and more accurate endonasal procedures. Some authors recommended the use of the endonasal approach for the inverted papilloma and the avoidance of any radical extranasal approach whenever possible13,14.
In our experience, 37.5% (three patients) were submitted to radical extranasal approach (maxilloethmoidal sinusectomy by medial facial degloving); 25% (two patients) were submitted to a limited extranasal approach (CaldwellLuc); and 37.5% (three patients) were submitted to endoscopic endonasal resection.
We believe that the choice of approach is closely correlated to the surgeon's experience with regards to the localization and size of the tumor. One should use the endonasal approach for smaller and less invasive lesions and use the extranasal approach (either combined or not) for cases that need wider safety margins.
Lawson et al.10 recommended conservative surgery for those lesions limited to the inferior and middle concha or those in the middle meatus area with minimum extension towards the anterior ethmoid or maxillary antrum. However, for lesions involving supraorbital cells, perilachrymal cells, frontal sinus and cribriform lamina this approach is contraindicated because, due to their localization, they provide poor visibility.
The literature shows varying recurrence rates of inverted papilloma when considering conservative approaches (an average of 60%). In radical approaches the average is 16%9.
In our study, we did not see any recurrence of inverted papilloma, although we had one case of inflammatory polyposis. However, we must consider that our follow-up time was short: from one to 47 months, with a mean of 18 months.
Malignancy rates described in literature vary from 5% to 13%, mean 9.2%9. In our study, no malignant transformations occurred.
CONCLUSIONAfter analyzing the results, we concluded that inverted papilloma is a benign type tumor, originated in 62.5% of the cases in the lateral nasal wall; the major incidence was in men within a mean age of 61.5 years. The main pre-op complaint was nasal obstruction.
Surgical approach varied according to location and size of lesion, as well as to experience of the surgeon. There has been no recurrence of inverted papilloma up to present. We did not find malignant degeneration at histology analysis.
REFERENCES1. BATSAKIS, J.G. - Tumors of the Head and Neck. Baltimore, The Williams & Wilkins Company, 1979.
2. BERNAUER H.S., et al. - Inverted Papillomas of the Paranasal Sinuses and the Nasal Cavity: DNA Indices and HPV Infection. Am J. Rhinol, 11(2):155-60, 1997.
3. BUCHWALD C. MD, et al. - Human Papillomavirus (HPV) in Sinonasal Papillomas: A Study of 78 Cases Using in Situ Hybridization and Polymerase Chain Reaction. Laryngoscope 105: 66-70, 1995.
4. BUCHWALD C. MD, et al. - Sinonasal Papillomas: A Report of 82 Cases in Copenhagen County, including a Longitudinal Epidemiological and Clinical Study. Laryngoscope 105:72-8, 1995.
5. CHEF LW.J. & SETHI D.S. - The Endoscopic Management Of Sinosal Inverted Papillomas. Clin. Otolaryngol. 24:61-6, 1999.
6. GRAHAM S.M: MD, et al. - Management Of inverted Papilloma. Head & Neck: 148-51, 1995.
7. GUICHARD C. MD, et al. - Epithelial Cell Proliferation, Apoptosis, and Apoptosis Inhibition in inverted papillomas. Laryngoscope 108:716-9, 1998.
8. Hwang, S.C. MD; Yang, S.H. MD; Hong, K.M. MD. - Detection of Human Papillomavirus in Sinonasal Inverted Papillomas Using Polymerase Chain Reaction (PCR). Am J. Rhinol 12:363-6, 1998.
9. LAWSON, W., et al. - Inverted Papilloma: A Report of 112 Cases. Laryngoscope 105: 282-8, 1995.
10. LAWSON, W.; Biller, H.F.; Jacobson, A. & Som, P. - The role of conservative surgery in the management of inverted papilloma. Laryngoscope 93:148-55, 1983.
11. MACDONALD M.R. MD, et al. - A Majority of Inverted Sinonasal Papillomas Carries Epstein-Barr Virus Genomes. Cancer 75(9):2307 11, 1995.
12. RAVEH, E.; FEINMESSER, R.; SHPITZER, T. et al. - Inverted papilloma of the nose and paranasal sinuses: A study of 56 cases and review of the literature. Isr J Med sci 32:1163-7, 1996.
13. SHAM C.L. et al. - Endoscopic resection of inverted papilloma of the nose and paranasal sinuses. J Laryngol Otol. 112:758-64, 1998.
14. THALER E.R. MD et al. - Endoscopically Assisted Anterior Cranial Skull Base Resection of Sinonasal Tumors. Am J. Rhinol 13(4):303 9, 1999.
1 Master in Otorhinolaryngology and Head and Neck Surgery, Doctorate studies under course, Universidade Federal de São Paulo - Escola Paulista de Medicina; Head of the Sector of Rhinology, Service of Otorhinolaryngology at Hospital do Servidor Público Estadual de São Paulo - Francisco Morato de Oliveira.
2 Assistant Physician, Service of Otorhinolaryngology, Hospital do Servidor Público Estadual de São Paulo - Francisco Morato de Oliveira.
3 Resident Physician, Service of Otorhinolaryngology, Hospital do Servidor Público Estadual de São Paulo - Francisco de Morato de Oliveira.
4 Resident Physician, Service of Pathological Anatomy, Hospital do Servidor Público Estadual de São Paulo - Francisco de Morato de Oliveira.
Address correspondence to: Erich Christiano Madruga de Melo - Rua Borges Lagoa, 1565, apt°. 10 - Vila Clementino - 04038-034 São Paulo /SP
Tel: (55 11) 9408-0554 - E-mail: erichmelo@uol.com.br
Service of Otorhinolaryngology, Hospital do Servidor Público Estadual de São Paulo - Francisco Morato de Oliveira, HSPE-FMO.
Article submitted on April 172, 2001. Article accented on June 18, 2001.


