INTRODUCTIONEosinophilic angiocentric fibrosis (EAF) is a rare affection that involves the sinonasal tract of young people, normally women, leading to fibrotic proliferation of nasal mucosa and obstructive symptoms of the upper airways. Less commonly, the disease may also affect the subglottic laryngeal region. This condition was initially described by Roberts and McCann in 1985, who noted that a disease of unknown etiology affected the nasal mucosa in two patients and the subglottic region of a third patient. The authors thought it was a variant of facial granuloma 1. In the literature, there are only 13 cases reported to present, nine women and four men.
Histologically, EAF is characterized by perivascular infiltrate rich in eosinophils, plasmocytes and histiocytes, which progress to perivascular concentric fibrosis. Differently from what happens in other nasal granulomatous diseases, such as Wegener's granulomatosis, sarcoidosis and tuberculosis, among others, necrotizing vasculitis processes, fibrinoid necrosis, intravascular thrombosis or granuloma formations are absent in such cases 1. Fibrotic processes affecting the nasal septum end up leading to nasal obstruction, whereas laryngeal affection may cause subglottic stenosis 2.
The nasal disease affects both the septum mucosa and the lateral wall of the nasal cavity, which also helps to differentiate the EAF from midline granulomatous diseases that tend to spare the lateral wall. Moreover, in EAF there are no mucosa ulcerations such as in granulomatosis 2.
Subjects with EAF do not experience systemic impairment. Owing to the existing significant perivascular eosinophilic infiltrate, the possibility of a cause of allergic nature has been made, but no confirmation has been reached so far. Different therapeutic attempts have already been made for this disease, but most authors mentioned surgery as the treatment of choice, even though there may be multiple recurrences. Thus, some forms of adjuvant treatment were attempted, to try to prevent recurrence and improve clinical control of the disease, such as use of corticoids by local or systemic infiltration. None of these forms of clinical treatment demonstrated any good results. EAF is to present a disease treated by controversial approaches 3, 4.
CASE REPORTPatient H.P.A., aged 62 years, male, complaining of long lasting bilateral nasal obstruction. He did not report pain, episodes of sinusitis or epistaxis. The physical examination showed marked septal deviation to the right in addition to significant thickness of anterior septal region, compromising bilateral nasal permeability. nasofibroscopy showed presence of a polyp of benign aspect, blocking the right middle meatus.
The complementary exams performed were:
1- Paranasal Sinuses Computed Tomography (CT scan) that showed septal deviation and thickness, associated with diffuse velamentum of right maxillary sinus with blockage of ostiomeatal complex on the same size (Figure 1).
2- Lab tests: complete blood count and hemosedimentation rate within the normal range; dosages of IgA, IgG, IgM within the normal range, except for IgE that was significantly increased; specific IgE (RAST) for home dust was not detected; anti-neutrophil cytoplasmatic antibody (ANCA) dosage was non-reactive; skin reaction by PPD was non-reagent.
The patient was submitted to nasal surgical procedure in which we observed thickened anterior cartilaginous septum, with fibrotic tissue aspect. We proceeded with detachment of mucosa with nasal septum and we removed most of the fibrotic structure of the septum to reduce its thickness. We also conducted right uncinectomy, polypectomy and right anterior ethmoidectomy via endoscopic approach.
The material removed from the nasal septum was sent to histopathological exam whose report revealed: dense connective tissue with foci of chronic lymphoplasmocytarian and eosinophilic inflammatory reaction. The tissue is sometimes along the adjacent cartilaginous tissues and shows foci of calcifications. In some areas we can see blood vessels with concentric fibrosis with onion peel aspect, filled with inflammatory infiltrate rich in eosinophils (Figure 2).
The patient progressed well in the postoperative period, without further complications, except for the formation of nasal crusts that were easily removed with sterile solution lavage for approximately 30 days. In mid-postoperative term, the patient presented mild nasal bleeding that improved after temporary discontinuation of topical drugs with corticoids. After 24 months of follow-up, there were no signs of recurrence of nasal thickness nor nasal polyps.
DISCUSSIONEosinophilic angiocentric fibrosis is a rare disease in which there is submucous fibrosis of sinusal tract and it is less common in the laryngeal subglottic region 1, 5. Patients affected by it may present mass in the nasal cavity, maxillary pain, epistaxis, repetitive sinusitis, rhinorrhea, or more commonly, long lasting obstructive nasal symptoms 3, 6. Authors that initially described the disease said it was a variant of facial granuloma, which is not a consensus in the literature 1. To our knowledge, there have been only 13 cases described in the world medical literature to present. EAF affects preferably young and middle-aged women with an incidence ratio of 4:9 male: female, ages ranging from 25 to 64 years, mean age of 44.6 years.
Etiology of EAF is not well known. The presence of eosinophils in lesions and the clinical history of allergic rhinitis in at least six patients already reported suggested a possible allergic cause 7. Previous nasal trauma, including septal surgery, was raised by Matai et al.7. Thompson et al.3, however, reported three cases without association with allergy or nasal trauma. Thus, the association with allergic disease or nasal trauma can be a mere coincidence. To present, there is also no association of EAF with nasal polyposis 1-9.
The diagnosis of EAF can be suspected in patients with history of long-time nasal obstruction that present nasal cavity mass (located at the septum or lateral cartilage, in special). This aspect may be visualized as septal widening in imaging tests. Diagnostic confirmation, however, can only be made through histopathologic exam 7, 8.
Histology shows lesions in different stages of evolution, from initial inflammatory process with vascular proliferation and dense lymphocyte infiltrate, with plasmocytes, neutrophils and especially eosinophils, to areas of perivascular fibrosis with thickness of vessel walls by proliferation of fibroblasts 3, 8. There is no granulomatous reaction, vascular necrotic process or presence of lymphoid follicles 8. Immunohistochemical exam is not mandatory for the diagnosis, but when it is conducted, it confirms the inflammatory nature of EAF, differentiating it from neoplasms 7.
As to imaging exams, simple x-ray shows nonspecific aspects such as paranasal sinuses opacification, bone sclerosis and focal destruction of bone tissues of nasal cavity or maxillary sinus walls. CT scan may be used to assess the extension of the lesions, both nasal and laryngeal, as well as the grade of involvement of anatomical structures 7.
Differential diagnosis of EAF includes Wegener's granulomatosis, Kimura's disease, angiolymphoid hyperplasia, myofibroblastic tumor (inflammatory pseudotumor), facial granuloma, Churg-Strauss syndrome, sarcoidosis, Sjogren's syndrome, infectious granulomatous disease such as tuberculosis and Hansen's disease, in addition to neurogenic neoplasms (schwannoma), vascular affections (angiofibroma) and mesenchymal abnormalities (fibroma, fibrosarcoma, nodular fasciitis, fibromatosis)1-9. To Thompson et al.3, the main differential diagnosis would be Wegener's granulomatosis, Churg-Strauss syndrome and fibrosarcoma. The different clinical manifestations combined with histological, laboratory and immunohistochemical findings help differentiate these rare diseases one from the other 3.
Thus, some exams can be ordered to these patients who have suspicion of nasal granulomatous diseases: differential count of blood cells (significant eosinophilia is detected in Churg-Strauss syndrome); hemosedimentation rate (which is increased in granulomatosis and in collagenosis, but it may be normal in EAF); ANCA (which may be increased in Wegener's granulomatosis); simple chest x-ray to investigate sarcoidosis and tuberculosis; Mantoux reaction - PPD for tuberculosis. Moreover, to investigate the allergic affection, other tests may be ordered for serum IgE and radio allergosorbent testing (RAST) to detect specific IgE antibodies against house and fungal antigens 1-9.
Histologically, most lesions can be differentiated among each other. In Churg-Strauss syndrome, there is vessel fibrinoid vasculitis, intravascular thrombosis and formation of granulomas affecting not only the sinonasal tract, but also other sites such as the kidneys and the lungs 2,3. Loane et al.9 reported the case of a patient with Wegener's granulomatosis and EAF simultaneously, suggesting a possible mechanism similar to pathogenesis of both diseases. Kimura's disease and inflammatory pseudotumor may be differentiated from EAF by the fact that in these lesions the inflammatory infiltrate is mixed and there is no significant fibrosis. Moreover, in Kimura's disease, there are dense lymphoid aggregates with well differentiated germinate centers. In facial granuloma, conversely, there is polymorphous inflammatory infiltrate with frequent vasculitis leading to thrombosis and fibrotic necrosis of vessel walls, in addition to extravascular leak of erythrocytes. Of all cases reported in the literature, only two had simultaneous manifestations of facial granuloma and EAF. In EAF there is characteristic concentric perivascular fibrosis, which is not found in other pathologies, in addition to not having vascular necrosis and giant cell granulomas 3, 6.
EAF treatment is mainly surgical for most authors, and it may require different surgical interventions, conveying a recurrent aspect to the disease 1-10. Topical or systemic corticoids or dapsone have been used as supporting therapy, but without satisfactory results 1-10. Cytotoxic agents have not been used so far, and we do not know whether they can provide benefits to the control of the disease 3.
CLOSING REMARKSThis case report tried to raise awareness of Otorhinolaryngologists about this rare affection. EAF should be part of the differential diagnosis of nasal granulomatous and neoplastic diseases. It is a disease of insidious course that ends up causing essentially obstructive symptoms of the upper airways. The definite diagnosis is based on histological aspects. To present, the only advocated treatment is essentially surgical, even though it is recognized by its post-surgical recurrent aspect.
REFERENCES1. Roberts PF, McCann BG. Eosinophilic angiocentric fibrosis of the upper respiratory tract: a mucosal variant of granuloma faciale? A report of three cases. Histopathology 1985; 9: 1217-25.
2. Burns BV, Roberts PF, Path FRC et al. Eosinophilic angiocentric fibrosis affecting the nasal cavity. A mucosal variant of the skin lesion granuloma faciale. J Laryngol Otol 2001; 115: 223-6.
3. Thompson LD, Heffner DK. Sinonasal tract Eosinophilic angiocentric fibrosis. Am J Clin Pathol. 2001; 115(2): 243-8.
4. Roberts PF, McCann BG. Eosinophilic angiocentric fibrosis of the upper respiratory tract: a postscript. Histopathology 1997; 3: 385-6.
5. Fageeh NA, Mai KT, Odell PF. Eosinophilic angiocentric fibrosis of the subglottic region of the larynx and upper trachea. J Otolaryngol 1996; 25(4): 276-8.
6. Pereira EM, Millas I, Reis-Filho JS et al. Eosinophilic angiocentric fibrosis of the sinonasal tract: report on the clinicopathologic features of a case and review of the literature. Head Neck 2002; 24(3): 307-11.
7. Matai V, Baer S, Barnes S, Boxer M. Eosinophilic angiocentric fibrosis. J Laryngol Otol 2000; 114(7): 563-4.
8. Loane J, Jaramillo M, Young HA, Kerr KM. Eosinophilic angiocentric fibrosis and Wegener's granulomatosis: a case report and literature review. J Clin Pathol 2001; 54(8): 640-1.
9. Owa AO, Boyle S, Gallimore AP. Eosinophilic angiocentric fibrosis as a cause of nasal obstruction. Rhinology 2002; 40: 41-3.
10. Altemani AM, Bem ZP, Sakano E, Altemani JM. Eosinophilic angiocentric fibrosis of the nasal cavity. Mod Pathol 1997; 10(4): 391-3.
Our special thanks to Dr Emílio M. Pereira, pathologist at Laboratório Salomão e Zoppi for the performance of the histopathological analyses of the present study.
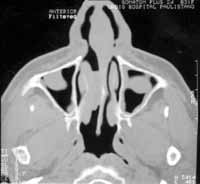 FIGURE 1-
FIGURE 1-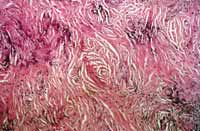 FIGURE 2-
FIGURE 2- 

